Articles
- Page Path
- HOME > J Prev Med Public Health > Volume 52(3); 2019 > Article
-
Original Article
Transformational Leadership and Depressive Symptoms in Germany: Validation of a Short Transformational Leadership Scale -
Max Leonhard Seegel1
 , Raphael M. Herr1
, Raphael M. Herr1 , Michael Schneider1, Burkhard Schmidt2
, Michael Schneider1, Burkhard Schmidt2 , Joachim E. Fischer1
, Joachim E. Fischer1 -
Journal of Preventive Medicine and Public Health 2019;52(3):161-169.
DOI: https://doi.org/10.3961/jpmph.19.002
Published online: May 12, 2019
- 5,190 Views
- 148 Download
1Mannheim Institute of Public Health, Social and Preventive Medicine, Medical Faculty Mannheim, Heidelberg University, Mannheim, Germany
2Department for Business, Work and Organizational Psychology, Applied University Fresenius, Heidelberg, Germany
- Corresponding author: Max Leonhard Seegel, MD Mannheim Institute of Public Health, Social and Preventive Medicine, Medical Faculty Mannheim, Heidelberg University, Mannheim 68167, Germany E-mail: maxseegel@gmx.de
Copyright © 2019 The Korean Society for Preventive Medicine
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
-
Objectives:
- The objective of the present study was to validate a shortened transformational leadership (TL) scale (12 items) comprising core TL behaviour and to test the associations of this shortened TL scale with depressive symptoms.
-
Methods:
- The study used cross-sectional data from 1632 employees of the overall workforce of a middle-sized German company (51.6% men; mean age, 41.35 years; standard deviation, 9.4 years). TL was assessed with the German version of the Transformational Leadership Inventory and depressive symptoms with the Hospital Anxiety and Depression Scale (HADS). The structural validity of the core TL scale was assessed with confirmatory factor analysis. Associations with depressive symptoms were estimated with structural equation modelling and adjusted logistic regression.
-
Results:
- Confirmatory factor analysis and structural equation modelling showed better model fit for the core TL than for the full TL score. Logistic regression revealed 3.61-fold (95% confidence interval [CI], 2.20 to 5.93: women) to 4.46-fold (95% CI, 2.86 to 6.95: men) increased odds of reporting depressive symptoms (HADS score >8) for those in the lowest tertile of reported core TL.
-
Conclusions:
- The shortened core TL seems to be a valid instrument for research and training purposes in the context of TL and depressive symptoms in employees. Of particular note, men reporting poor TL were more likely to report depressive symptoms.
- Depressive disorders are common in the general population [1] and the associated direct (e.g., medical treatment, transport and social services) and indirect (e.g., absenteeism, presenteeism, premature death) costs represent a high burden for the affected individuals, their families, employers, and social security systems [2,3]. Depressive symptoms, such as fatigue and diminished concentration, were found to impair work performance [4], and the absence of a clinical diagnosis does not exclude the presence of depressive symptoms in employees [5]. The disease is multifaceted, and the change from mild to severe depressive symptoms is gradual [6].
- In the workforce context, leadership is an important modifiable risk factor for an employee’s psychosocial well-being [7,8]. One of the most examined leadership styles is transformational leadership (TL) [9]. TL relies on promoting autonomy, personal empowerment, and team effectiveness, and has been associated with reduced depressive symptoms in employees [5,10,11]. According to Podsakoff et al. [12], TL is characterised by the following 6 behaviours: Intellectual stimulation (ISN): leaders encourage their followers to re-examine some of their assumptions about their work and to rethink how it can be performed. Providing individualised support (IS): leaders are concerned about their followers and care about their personal feelings and needs. Identifying and articulating a vision (AV): leaders aim to identify new opportunities for their company and inspire others with their vision of the future. Fostering the acceptance of group goals (FAG): leaders unite their employees to work together for a common goal by encouraging cooperation among employees. Providing an appropriate model (PAM): leaders set an example for their employees to follow which is consistent with their values. High-performance expectations (HPE): behaviour that shows leaders have high expectations for quality and performance on the part of the followers (Podsakoff et al. [12]). The authors also indicated that PAM, FAG, and AV could represent core TL behaviour with respect to mental health [12,13]. A study by Schmidt et al. [11] examining the association between TL and depressive symptoms indicated that these 3 core TL dimensions showed the strongest associations with TL.
- Various instruments have been implemented to assess TL, such as the often-utilized Multifactor Leadership Questionnaire (MLQ-5x) [14,15] and the Transformational Leadership Inventory (TLI) [12,16]. The TLI was developed in response to criticism of the factor structure of the MLQ-5x; it addresses the above-mentioned facets of TL with the advantage of relative brevity (23 items) and a more stable factor structure compared to the MLQ-5x (45 items). This instrument has been shown to predict work performance and commitment, and its results are consistent with a validation study of TL [13]. In contrast to shorter and unidimensional tools such as the Global Transformational Leadership Scale (7 items), which has already been used in research on TL and depressive symptoms [5], the TLI allows the different facets of TL [12,13,17] to be analysed. Recent research on TL and employee well-being has suggested the need to take into account the different dimensions of TL in this context [18]. The TLI seems therefore particularly suitable to assess the core TL scale.
- An abbreviated version of the TLI consisting only of those 12 core TL items would provide an economical, yet valid tool for research, and possibly also for interventions in the context of mental health, as it would focus on specific patterns of leadership behavior to be adressed in training and interventions.
- The aims of the present study were thus twofold: (1) to test the psychometric properties (structural validity and internal consistency) of TL, its dimensions, and core TL in a German population and (2) to test the correlation of core TL with depressive symptoms.
INTRODUCTION
- Study Population
- A random sample of 4027 employees, aged 20 years and above and representing an average distribution of age and gender, was drawn from the overall workforce of a middle-sized German company (n=7235). A total of 1632 employees (response rate, 41.5%) completed an online survey and provided written informed consent. Participants with missing values were excluded, which decreased the sample for the analysis to 1251 participants. The local ethical committee approved the study (2012-367N-MA).
- Questionnaires
- TL was evaluated using the validated German version of the TLI (Cronbach α=0.90) [12,13,16], which assessed ISN (3 items), IS (4 items), PAM (3 items), FAG (4 items), and AV (5 items). The HPE scale was excluded a priori for practical and theoretical reasons. HPE has been shown to have low internal consistency (Cronbach α=0.61 and α=0.62) in 2 previous studies by Podsakoff and colleagues [12,16] and a low correlation with the other facets of TL in a validation study [13]. In addition, it is not a proposed core dimension of TL [12,13]. Each item was rated on a 5-point Likert scale ranging from 1 (not at all) to 5 (all of the time). The mean was calculated for the subscores of the 5 TLI factors [13].
- Depressive symptoms were assessed using the validated German version of the Hospital Anxiety and Depression Scale (HADS; Cronbach α=0.88) [19,20]. The depression subscale with 7 items coded on a 4-point Likert scale was employed. The HADS is an established instrument used to predict symptom severity [21] and psychosocial and physical outcomes [22]. It has been shown to be valid in the general population with a high concurrent validity with other well-established tests, such as the Beck Depression Inventory, State-Trait Anxiety Inventory, Clinical Anxiety Scale, and Symptom Checklist-90 [21]. A sum score was computed (ranging from 0 to 21), with higher values indicating more depressive symptoms. For logistic regression, the cut-off for the presence of depressive symptoms was set at >8, as proposed in the literature [21].
- Additional covariates were age, gender, alcohol consumption, marital status, smoking habits, physical activity, body mass index, education, and job position (Table 1).
- Data Analyses
- The analytic strategy comprised 3 steps. First, the structural validity of the TLI score was assessed by confirmatory factor analysis (CFA). The TLI score was entered as a latent variable, defined by the respective subscores, which were inserted on a manifest item basis. Three models were tested:
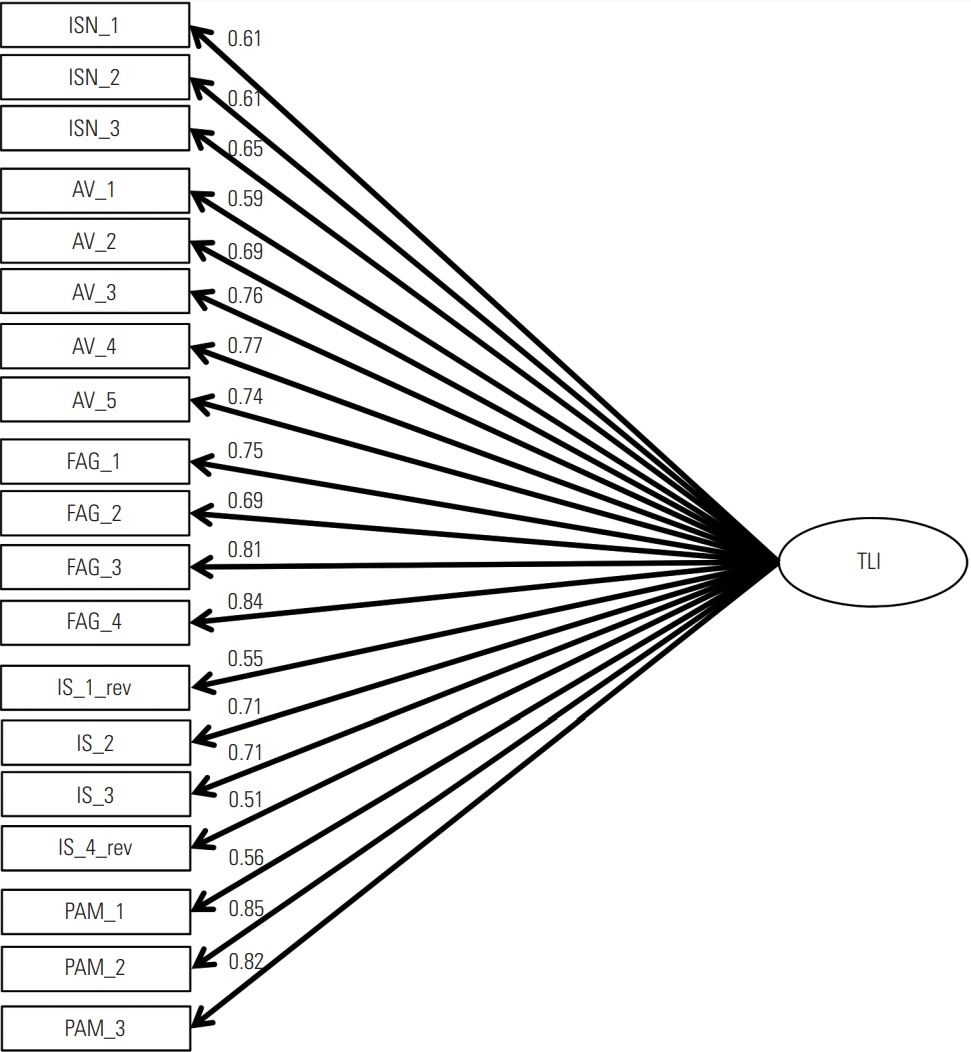
- (1) A 1-factor model in which all items loaded on the TLI score as the latent variable, omitting the subscores (Figure 1).
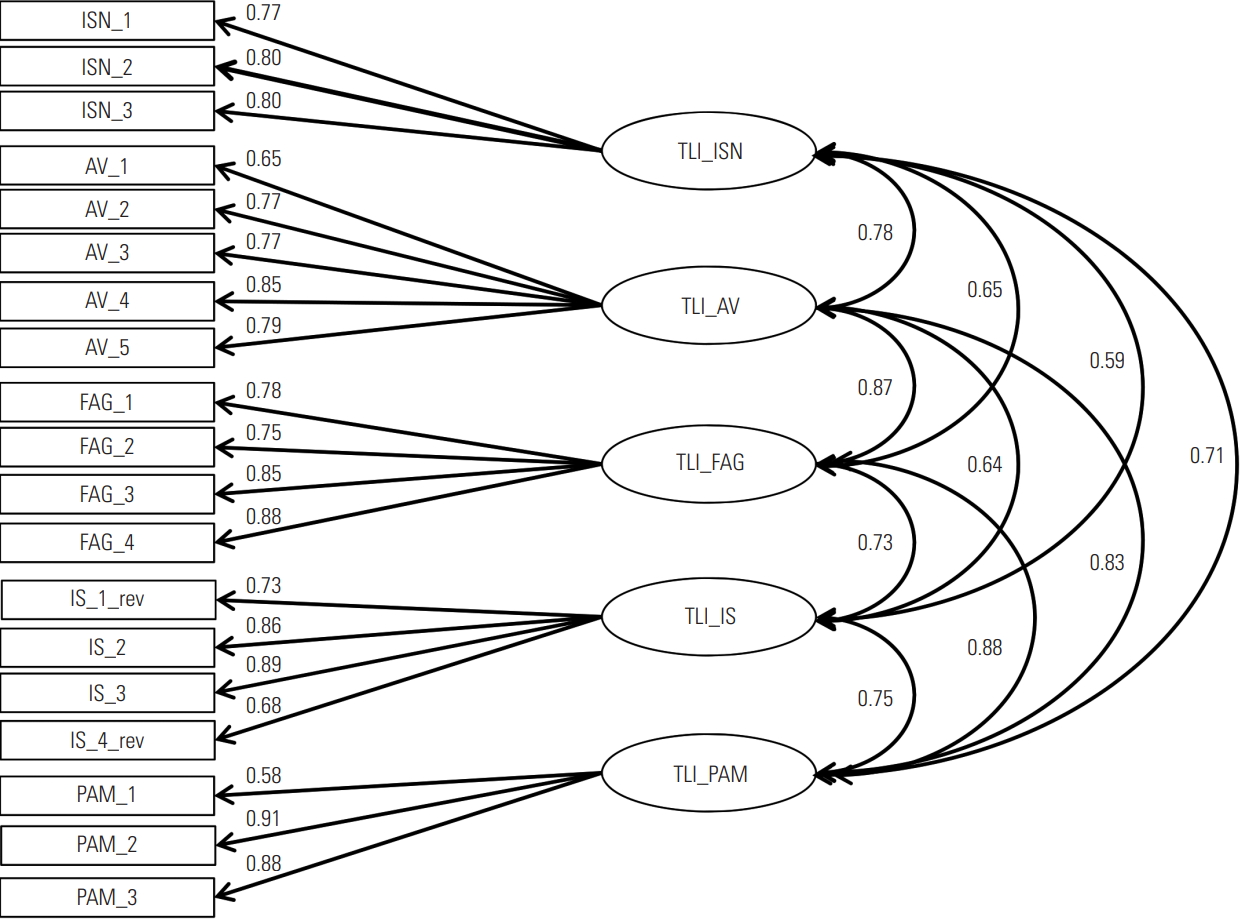
- (2) The full model in which all items loaded on the subscores (AV, FAG, PAM, IS, ISN), which then defined the TLI score as the latent variable (Figure 2).
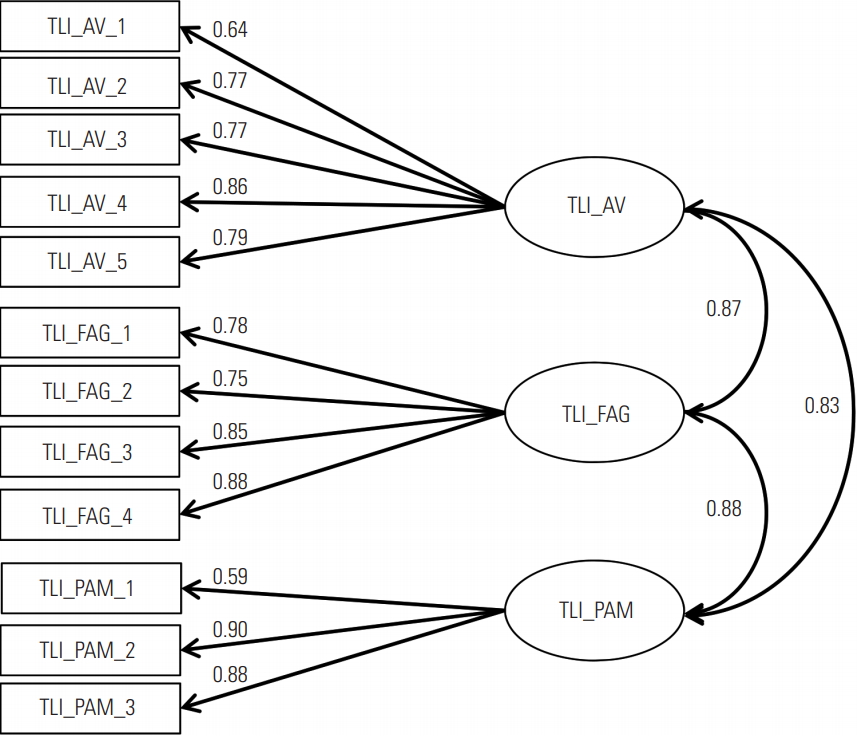
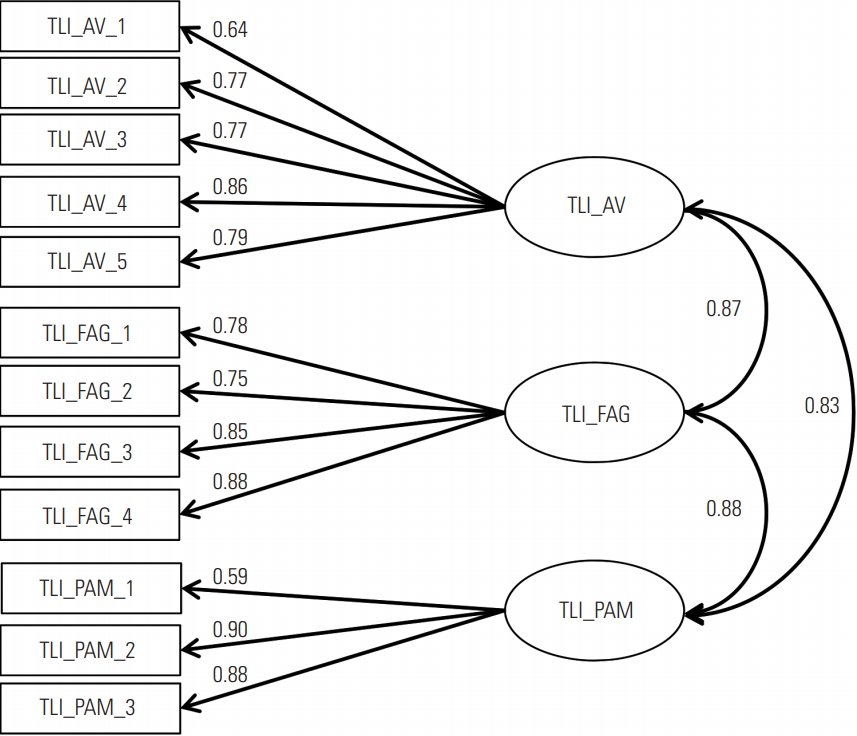
- (3) The core TL model, which only included the AV, FAG and PAM subscores loading on the TLI score (Figure 3).
- Second, item analysis of the core TL was performed using the Cronbach α, item-total correlation, and Cronbach α if an item is deleted.
- Third, the correlation of TL and depressive symptoms was assessed in 2 ways. First, structural equation modelling (SEM) with depressive symptoms as the outcome variable was used to compare both the full and the core TL model in relation to depressive symptoms. Additionally, both models were stratified for gender [23]. SEM analyses were carried out employing maximum likelihood estimation and bootstrapping (n=5000) to account for the non-normal distribution [24]. In accordance with current literature, the following fit indices to compare model fit among the 3 models were reported: chi-square (χ2), the Tucker-Lewis index/non-normed fit index (NNFI), the comparative fit index (CFI), and the root mean square error of approximation (RMSEA) [25,26]. The following cut-off values for good model fit have been proposed in the literature: CFI ≥0.95; NNFI ≥0.95; RMSEA <0.5 [25].
- Second, logistic regression models were constructed to quantify the associations between TL and depressive symptoms for the full and the core TL models and their respective scores. Analyses were adjusted for the following a priori identified relevant confounders: age, alcohol consumption, body mass index, marital status, smoking, education, gender, physical activity, and job position. The core TL was split into tertiles, using high TL as the reference group. Here, too, analyses were additionally stratified for gender [27,28]. All analyses were carried out using SPSS and Amos version 24.0 (IBM Corp., Armonk, NY, USA).
METHODS
- Participant Characteristics
- Approximately half the participants were men (52.7%), with an average age of 41.35 years (standard deviation, 9.41 years) (Table 1). The majority of the participants were married (60.1%), had received higher education (general qualification for university entrance) (59.8%), and worked in white-collar jobs (62.5%).
- Structural Validity
- Due to the exclusion of missing values, the sample used for CFA consisted of 1251 participants. The model fit for the 1-factor model (Figure 1) was not acceptable (χ2=19 025.052, df= 912, p<0.001; CFI=0.82; NNFI=0.79; RMSEA=0.05). The model fits for the full model (χ2=2636.19, df=852, p<0.001; CFI= 0.96; NNFI=0.96; RMSEA=0.02) and for the core TL model (χ2= 1313.38, df=306, p<0.001; CFI=0.97; NNFI=0.96; RMSEA= 0.03) were acceptable. Standardised regression coefficients for both the full model (Figure 2) and the core TL model (Figure 3) showed the highest associations between the AV, FAG, and PAM factors (FAG-PAM, 0.88; AV-PAM, 0.83; and AV-FAG, 0.87).
- Item Analysis
- The core TL showed good internal consistency. The Cronbach α was 0.94, with an item-total correlation ranging from 0.55 to 0.81. The Cronbach α of the core TL did not improve after deletion of any item. Regarding the sub-dimensions, for AV, the Cronbach α was 0.88 and the item-total correlation was 0.62 or higher. The Cronbach α for FAG was 0.89, and the item-total correlation was 0.72 or higher. For PAM, the Cronbach α was 0.83, and the item-total correlation varied from 0.55 to 0.77.
- Correlation of Transformational Leadership With Depressive Symptoms
- The comparison of the relationship between TL and depressive symptoms for the full model and the core TL model was performed with 2 statistical techniques: SEM and logistic regression analyses.
- In the SEM analyses, the relationship between TL and depressive symptoms was similar for both models (βfull model=-0.35; βcore TL model=-0.34). The lowest regression weights were found for ISN and IS, with β values of 0.76 and 0.77. Both the full model and the core TL model showed acceptable data fit (full model: χ2=15 510.94, df=990, p<0.001; CFI=0.95; NNFI=0.95; RMSEA=0.03; core TL model: χ2=1398.07, df=372, p<0.001; CFI=0.97; NNFI=0.96; RMSEA=0.03). The core TL model fit the data better than the full model (Δχ2=4112.87, df=618, p<0.001). The models stratified for gender indicated that the association between TL and depressive symptoms was stronger among men in the full and the core TL models (βfull-model=-0.41; βcore TL model=-0.40) than for women (βfull-model=-0.26; βcore TL model=-0.26).
- Table 2 shows the results for the logistic regression models. For the full and the core TL models, individuals within the lowest TL tertile were 3.36 to 4.50 times more likely to experience depressive symptoms than those in the highest tertile (odds ratio [OR], 3.98; 95% confidence interval [CI], 2.87 to 5.52; p< 0.01 and OR, 4.50; 95% CI, 3.23 to 6.27; p<0.01). This association remained consistent for all subscores. The association in the core TL model was strongest for men, in both the core TL and the full models (men: OR, 4.46; 95% CI, 2.86 to 6.95; p< 0.01 and OR, 5.10; 95% CI, 3.20 to 8.14; p<0.01; women: OR, 3.61; 95% CI, 2.20 to 5.93; p<0.01 and OR, 3.94; 95% CI, 2.43 to 6.39; p<0.01).
RESULTS
- The present study is, to the best of our knowledge, the first to examine the relationship between TL and depressive symptoms while taking into consideration the different components of TL and core TL. The fit of the CFA for the full model was acceptable, and still better for the core TL model. In the full model, the AV, FAG, and PAM subscores had the highest loadings on TL, and reducing the model to the core TL did not significantly alter the β values. Item analyses indicated good internal consistency within core TL. The SEM analyses revealed a significant association between lower levels of core TL and more depressive symptoms. Logistic regression analyses based on TL split in tertiles further suggested a dose-response relationship for both the full and the core TL model, indicating a positive linear relationshp. In summary, 3 of the 5 TL dimensions (core TL) explained most of the variance in the relationship between TL and depressive symptoms.
- Podsakoff et al. [12] suggested certain facets of TL to be indicators of an underlying core TL behaviour (AV, FAG, PAM). A German validation study confirmed these findings, as those facets again showed the highest correlations with the measure for TL [13]. In a recent meta-analysis, Harms et al. [29] further suggested that the more abstract aspects of TL, such as ISN and HPE, are less important for the effect of TL on mental health than the other, more “relationship-based” components. This study provides further support for that proposal.
- Several mechanisms might explain the mental health effects of TL. Leadership behaviour that promotes a clear and inspiring vision of the future (AV) can induce positive appraisal and reduce maladaptive behaviour in subordinates [30] as demands are perceived as a challenge rather than a menace [31]. It could also lead to a more meaningful work environment, which presents another contextual resource [5,17].
- The effects of shared vision and sense of community promoted by a leader who unites his/her followers probably even extend further. Those personal qualities comprise encouraging cooperation, working towards common goals (FAG), and setting an example which is consistent with one’s own values (PAM). This behaviour can result in a social support culture within a group [30], which is another crucial protective contextual resource for employees [32-35].
- ISN, in contrast, which requires re-examining assumptions about and re-thinking procedures related to one’s work, can induce stress and result in uncertainty, especially when it requires the employee to back opinions with reasons [36]. For some employees, “thinking out of the box” might be beneficial, but doing so also has been linked to burnout and negative well-being [36,37]. In the present study, though, ISN did not contribute significantly to the link between TL and depressive symptoms.
- Even though it seems plausible that the IS of an employee’s personal needs and feelings should have a positive impact on stress and, eventually, depressive symptoms, this facet played a less important role in the present study.
- Another interesting finding relates to the stronger association of TL and depressive symptoms among men than among women. There are no prior reports on this gender difference, as in both previous studies, women were highly overrepresented (85% and 93%, respectively) [5,10]. In general, most studies and meta-analyses on TL and mental health have not reported gender differences. Further studies are needed to explore the influence of gender on the relationship between TL and depressive symptoms.
- The present study supports previous findings on the inverse correlation of TL and depressive symptoms. Beyond that, it is the first study to examine the effects of the different dimensions of TL on depressive symptoms. On this basis, we validated a shortened, yet 3-dimensional, version of the TLI, which could represent a useful instrument for research and training purposes.
- Nevertheless, several limitations of this study need to be addressed. First, its cross-sectional design does not allow any conclusions to be drawn about potential causal relationships between TL and depressive symptoms. Second, our data were obtained from a German company. Thus, the generalizability of our findings to overall working populations in and beyond Germany is limited. Moreover, a common issue in workplace studies is healthy worker bias (selection of healthy workers), which may influence the association between TL and depressive symptoms, as employees who experience poor leadership might be more likely to quit their job or be absent because of depression. This, in turn, would lead to underestimation of the association. In addition, HPE was not measured in this study. The HPE dimension has been shown to have low internal consistency in 2 separate populations and a low correlation with other TL scales [13]. The conception of core TL in our study was based on theoretical considerations and supported by results of different studies [11-13]. However, we cannot completely rule out the possibility that including HPE in our study could have had an influence on our results.
- In addition to leadership, other psychosocial work factors at the workplace are associated with depressive symptoms, such as bullying, psychological demands, low support or conflicts with colleagues, unfavourable social climate, job insecurity, and a long work week [38]. In addition, stressful life events or chronic conditions outside the workplace might also play an important role. Further studies are needed to examine the independent effect of (core) TL on depressive symptoms.
- In conclusion, it is feasible to implement the shortened core TL, which consists of 12 items, as opposed to 19 items in the full version, as an instrument for research and training purposes in the context of TL and depressive symptoms in employees. Using this instrument, we were able to replicate the inverse correlation between TL and depressive symptoms. Additionally, we found that men who reported poor TL were at an especially increased risk of experiencing a higher number of depressive symptoms.
DISCUSSION
-
CONFLICT OF INTEREST
The authors have no conflicts of interest associated with the material presented in this paper.
Notes
ACKNOWLEDGEMENTS


Values are presented as odds ratio (95% confidence interval).
TL, transformational leadership; HADS, Hospital Anxiety and Depression Scale; AV, identifying and articulating a vision; PAM, providing an appropriate model; FAG, fostering the acceptance of group goals.
1 Models were adjusted for age, alcohol consumption, body mass index, marital status, smoking, education, gender, physical activity and job position.
- 1. Jacobi F, Wittchen HU, Holting C, Höfler M, Pfister H, Müller N, et al. Prevalence, co-morbidity and correlates of mental disorders in the general population: results from the German Health Interview and Examination Survey (GHS). Psychol Med 2004;34(4):597-611ArticlePubMed
- 2. Luppa M, Heinrich S, Angermeyer MC, König HH, Riedel-Heller SG. Cost-of-illness studies of depression: a systematic review. J Affect Disord 2007;98(1-2):29-43ArticlePubMed
- 3. Simon GE, Barber C, Birnbaum HG, Frank RG, Greenberg PE, Rose RM, et al. Depression and work productivity: the comparative costs of treatment versus nontreatment. J Occup Environ Med 2001;43(1):2-9ArticlePubMed
- 4. Lerner D, Henke RM. What does research tell us about depression, job performance, and work productivity? J Occup Environ Med 2008;50(4):401-410ArticlePubMed
- 5. Perko K, Kinnunen U, Feldt T. Transformational leadership and depressive symptoms among employees: mediating factors. Leadersh Organ Dev J 2014;35(4):286-304Article
- 6. Prisciandaro JJ, Roberts JE. A taxometric investigation of unipolar depression in the national comorbidity survey. J Abnorm Psychol 2005;114(4):718-728ArticlePubMedPDF
- 7. Kuoppala J, Lamminpää A, Liira J, Vainio H. Leadership, job well-being, and health effects--a systematic review and a meta-analysis. J Occup Environ Med 2008;50(8):904-915ArticlePubMed
- 8. Schmidt B, Loerbroks A, Herr RM, Wilson MG, Jarczok MN, Litaker D, et al. Associations between supportive leadership and employees self-rated health in an occupational sample. Int J Behav Med 2014;21(5):750-756ArticlePubMedPDF
- 9. Judge TA, Piccolo RF. Transformational and transactional leadership: a meta-analytic test of their relative validity. J Appl Psychol 2004;89(5):755-768ArticlePubMedPDF
- 10. Munir F, Nielsen K, Carneiro IG. Transformational leadership and depressive symptoms: a prospective study. J Affect Disord 2010;12089(1-3):235-239Article
- 11. Schmidt B, Loerbroks A, Herr R, Litaker D, Wilson M, Kastner M, et al. Psychosocial resources and the relationship between transformational leadership and employees’ psychological strain. Work 2014;49(2):315-324ArticlePubMed
- 12. Podsakoff PM, MacKenzie SB, Moorman RH, Fetter R. Transformational leader behaviors and their effects on followers’ trust in leader, satisfaction, and organizational citizenship behaviors. Leadersh Q 1990;1(2):107-142Article
- 13. Heinitz K, Rowold J. Psychometric properties of a German adaptation of the Transformational Leadership Inventory (TLI) by Podsakoff. Ger J Work Organ Psychol 2007;51(1):1-15. (German)
- 14. Felfe J. Validation of a German version of the “Multifactor Leadership Questionnaire” (MLQ Form 5 x Short) by Bass and Avolio (1995). Ger J Work Organ Psychol 2006;50(2):61-78. (German)
- 15. Bass BM. Two decades of research and development in transformational leadership. Eur J Work Organ Psychol 1999;8(1):9-32Article
- 16. Podsakoff PM, MacKenzie SB, Bommer WH. Meta-analysis of the relationships between Kerr and Jermier’s substitutes for leadership and employee job attitudes, role perceptions, and performance. J Appl Psychol 1996;81(4):380-399ArticlePubMedPDF
- 17. Nielsen K, Randall R, Yarker J, Brenner SO. The effects of transformational leadership on followers’ perceived work characteristics and psychological well-being: a longitudinal study. Work Stress 2008;22(1):16-32Article
- 18. Arnold KA. Transformational leadership and employee psychological well-being: a review and directions for future research. J Occup Health Psychol 2017;22(3):381-393ArticlePubMedPDF
- 19. Hinz A, Schwarz R. Test information. Diagnostica 2002;48(2):112-113. (German)Article
- 20. Zigmond AS, Snaith RP. The hospital anxiety and depression scale. Acta Psychiatr Scand 1983;67(6):361-370ArticlePubMed
- 21. Bjelland I, Dahl AA, Haug TT, Neckelmann D. The validity of the Hospital Anxiety and Depression Scale. An updated literature review. J Psychosom Res 2002;52(2):69-77ArticlePubMed
- 22. Herrmann C. International experiences with the Hospital Anxiety and Depression Scale--a review of validation data and clinical results. J Psychosom Res 1997;42(1):17-41ArticlePubMed
- 23. Stewart WF, Ricci JA, Chee E, Hahn SR, Morganstein D. Cost of lost productive work time among US workers with depression. JAMA 2003;289(23):3135-3144ArticlePubMed
- 24. Sainani KL. Dealing with non-normal data. PM R 2012;4(12):1001-1005ArticlePubMed
- 25. Hooper D, Coughlan J, Mullen M. Structural equation modelling: guidelines for determining model fit. Electron J Bus Res Methods 2008;6(1):53-60
- 26. Hu LT, Bentler PM. Cutoff criteria for fit indexes in covariance structure analysis: conventional criteria versus new alternatives. Struct Equ Modeling 1999;6(1):1-55Article
- 27. Yusuf S, Hawken S, Ounpuu S, Dans T, Avezum A, Lanas F, et al. Effect of potentially modifiable risk factors associated with myocardial infarction in 52 countries (the INTERHEART study): case-control study. Lancet 2004;364(9438):937-952ArticlePubMed
- 28. Herr RM, Li J, Bosch JA, Schmidt B, DeJoy DM, Fischer JE, et al. Psychometric properties of a German organizational justice questionnaire (G-OJQ) and its association with self-rated health: findings from the Mannheim Industrial Cohort Studies (MICS). Int Arch Occup Environ Health 2014;87(1):85-93ArticlePubMedPDF
- 29. Harms PD, Credé M, Tynan M, Leon M, Jeung W. Leadership and stress: a meta-analytic review. Leadersh Q 2017;28(1):178-194ArticlePubMedPMC
- 30. Lyons JB, Schneider TR. The effects of leadership style on stress outcomes. Leadersh Q 2009;20(5):737-748Article
- 31. Wegge J, Shemla M, Haslam SA. Leader behavior as a determinant of health at work: specification and evidence of five key pathways. Ger J Hum Resour Manag 2014;28(1-2):6-23. (German)Article
- 32. Nielsen K, Daniels K. Does shared and differentiated transformational leadership predict followers’ working conditions and well-being? Leadersh Q 2012;23(3):383-397Article
- 33. Arnold KA, Turner N, Barling J, Kelloway EK, McKee MC. Transformational leadership and psychological well-being: the mediating role of meaningful work. J Occup Health Psychol 2007;12(3):193-203ArticlePubMedPDF
- 34. Zwingmann I, Wegge J, Wolf S, Rudolf M, Schmidt M, Richter P. Is transformational leadership healthy for employees? A multilevel analysis in 16 nations. Ger J Hum Resour Manag 2004;28(1-2):24-2513. (German)Article
- 35. Stansfeld SA, Fuhrer R, Head J, Ferrie J, Shipley M. Work and psychiatric disorder in the Whitehall II Study. J Psychosom Res 1997;43(1):73-81ArticlePubMed
- 36. Seltzer J, Numerof RE, BASS BM. Transformational leadership: Is it a source of more burnout and stress? J Health Hum Resour Adm 1989;12(2):174-185
- 37. Zineldin M, Hytter A. Leaders’ negative emotions and leadership styles influencing subordinates’ well-being. Int J Hum Resour Manag 2012;23(4):748-758Article
- 38. Theorell T, Hammarström A, Aronsson G, Träskman Bendz L, Grape T, Hogstedt C, et al. A systematic review including meta-analysis of work environment and depressive symptoms. BMC Public Health 2015;15: 738ArticlePubMedPMCPDF
REFERENCES
Figure & Data
References
Citations

 KSPM
KSPM

 PubReader
PubReader ePub Link
ePub Link Cite
Cite