Articles
- Page Path
- HOME > J Prev Med Public Health > Volume 45(1); 2012 > Article
-
Original Article
Impact of Individual and Combined Health Behaviors on All Causes of Premature Mortality Among Middle Aged Men in Korea: The Seoul Male Cohort Study - Chul Woo Rhee1, Ji Young Kim1, Byung Joo Park1,2, Zhong Min Li3, Yoon-Ok Ahn1,3
-
Journal of Preventive Medicine and Public Health 2012;45(1):14-20.
DOI: https://doi.org/10.3961/jpmph.2012.45.1.14
Published online: January 31, 2012
1Department of Preventive Medicine, Seoul National University College of Medicine, Seoul, Korea.
2Medical Research Collaborating Center, Seoul National University Hospital, Seoul National University College of Medicine, Seoul, Korea.
3Institute of Radiation Effect & Epidemiology, Seoul National University Medical Research Center, Seoul, Korea.
- Corresponding author: Yoon-Ok Ahn, MD, PhD. 103 Daehak-ro, Jongno-gu, Seoul 110-799, Korea. Tel: +82-2-740-8322, Fax: +82-2-747-4830, (yoahn@snu.ac.kr)
- *Current affiliation: School of Public Health Sciences, Jilim University, Changchun, China
Copyright © 2012 The Korean Society for Preventive Medicine
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
-
Objectives
- The aim of this study was to evaluate and quantify the risk of both individual and combined health behaviors on premature mortality in middle aged men in Korea.
-
Methods
- In total, 14 533 male subjects 40 to 59 years of age were recruited. At enrollment, subjects completed a baseline questionnaire, which included information about socio-demographic factors, past medical history, and life style. During the follow-up period from 1993 to 2008, we identified 990 all-cause premature deaths using national death certificates. A Cox proportional hazard regression model was used to estimate the hazard ratio (HR) of each health risk behavior, which included smoking, drinking, physical inactivity, and lack of sleep hours. Using the Cox model, each health behavior was assigned a risk score proportional to its regression coefficient value. Health risk scores were calculated for each patient and the HR of all-cause premature mortality was calculated according to risk score.
-
Results
- Current smoking and drinking, high body mass index, less sleep hours, and less education were significantly associated with all-cause premature mortality, while regular exercise was associated with a reduced risk. When combined by health risk score, there was a strong trend for increased mortality risk with increased score (p-trend < 0.01). When compared with the 1-9 score group, HRs of the 10-19 and 20-28 score groups were 2.58 (95% confidence intervals [CIs], 2.19 to 3.03) and 7.09 (95% CIs, 5.21 to 9.66), respectively.
-
Conclusions
- Modifiable risk factors, such as smoking, drinking, and regular exercise, have considerable impact on premature mortality and should be assessed in combination.
- Assessing the combined impact of health-related behaviors is complex. Several studies have shown that specific health behaviors, such as smoking, current drinking, and physical inactivity are associated with poor health outcomes in Western countries, as well as in Korea [1-6]. Moreover, in the prevention of chronic diseases, these modifiable risk factors are an even greater concern [7,8]. In most studies, independent risks of health-related behaviors are evaluated using statistical adjustment for other risk factors and confounders. However, poor health behaviors and protective factors often coexist with one another. Thus, identifying independent risks of health behaviors and assessing them together, based on a combined impact, are both important.
- One way to assess the impacts of health behaviors is to evaluate their association with mortality. Morality is frequently used to quantify the extent of public health problems and to determine the relative importance of various causes of death. This enables a direct comparison between risk factors and protective factors, and even allows for the estimation of combined effects. To date, several studies have examined the combined effects of health behaviors on mortality in Western countries [9-12]. The EPIC-Norfolk prospective population study reported an increased risk of all-cause mortality by 4.04-fold (95% confidence intervals [CIs], 2.95 to 5.54) in people with no healthy behaviors as compared to those with four healthy behaviors [9]. Another study focused on dietary patterns and lifestyle factors among individuals aged 70 to 90 years, and reported that adherence to a Mediterranean diet and a healthy lifestyle was associated with a more than 50% lower rate of all-cause mortality [10]. The most recent study that evaluated the influence of combined health behaviors on mortality reported that, compared to those with no poor behaviors, persons with four poor health behaviors had a 3.49-fold increased risk for all-cause mortality [12].
- When quantifying the combined impact, counting number of poor and good health behaviors is common; however, this method is only possible under the assumption that the magnitudes of all poor and good health behaviors are equal. Realistically, the magnitude of their effects regarding mortality is not always equal [11,12]. Thus, weighting the effects of health behaviors by accounting for their magnitude seems more reasonable.
- Because most deaths occur among older persons, alternative measures, such as premature mortality, have been proposed to reflect mortality in younger age groups by weighting deaths occurring at younger ages more heavily than those occurring in older populations [13]. Despite its importance, few studies have been performed to evaluate the combined risks of health behaviors on premature mortality in Korea. Because well-known risk behaviors, such as smoking and alcohol consumption, have been studied predominantly in males in Korea, we examined the risk of both individual and combined health behaviors on premature mortality in middle aged men in Korea.
INTRODUCTION
- I. Study Cohort
- The design of the Seoul Male Cohort Study has been described previously [14-16]. The original cohort was recruited in January 1992. Criteria for the eligible population were males aged 40 to 59 years, residing in or near Seoul, who were beneficiaries of the Korea Medical Insurance Corporation (KMIC), and who were confirmed to be disease-free at a biennial health check-up conducted in 1990. KMIC, now known as the National Health Insurance Corporation (NHIC), covered all government employees, school teachers, and pensioners at the time of the study. For the baseline evaluation, a self-administered questionnaire survey was used with stratified cluster random sampling. Four strata of institutions, according to the size of their source population, were selected initially. Based on an estimated questionnaire response rate of 50%, 29 918 subjects were sampled in total. After mailing the 16-page questionnaire up to three times, 14 533 completed baseline surveys were collected with information regarding demographics, past medical history, family history, dietary habits, and life style characteristics.
- II. Assessment of Health Behaviors
- Age at entry was grouped into 5-year groups of 40 to 44, 45 to 49, 50 to 54, and 55 to 59 years. Smoking and alcohol behavior were divided into three categories: current, former, and never. Body mass index (BMI) was calculated as weight (kg) divided by squared height (m2), which was then classified according to the BMI classification recommended by the World Health Organization [17].
- For assessing physical activity, the question "In the past year, how many days a week have you spent on vigorous exercise or physical labor?" was asked. Based on the response, physical activity was categorized as none, 1 to 3 times, and ≥4 times. For sleep hours, respondents were asked to report the usual number of sleep hours, including naps. Education level response categories were no education, elementary school, middle school, high school, community college, university, and postgraduate. There were also questions about past medical history, including whether the subjects had diabetes mellitus or hypertension.
- III. Outcome Assessment
- Each cohort participant was followed from January 1, 1993 to December 31, 2008. Mortality data were collected annually using death certificates from the National Statistical Office. About 97% of deaths in Seoul are accompanied by death certificates issued by a doctor. Causes of death are given with the International Classification of Disease (ICD)-10 codes.
- To define premature death, life expectancy data for middle-aged men in 1992 from the National Statistical Office were used. In 1992, life expectancy was 31.54, 27.78, 23.27, and 19.49 for males aged 40, 45, 50, and 55 years, respectively [18]. Any cause of death before the life expectancy for their age group was defined as a premature death in this study.
- IV. Statistical Analyses
- Categorical variables are presented as numbers and percentages and continuous variables are presented as means and standard deviations. For evaluating associations and comparing differences between the two groups, a χ2 test or t-test was used, as appropriate. Univariate and multivariate Cox proportional hazards regression models were used to determine the hazard ratio of each risk behaviors. Variables with p-values <0.2 in the univariate analysis were selected as potential confounders for the multivariate model.
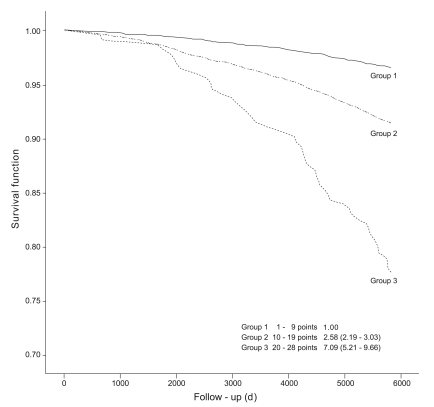
- Finally, to develop a risk stratification algorithm to assess combined health behaviors in relation to all-cause premature mortality, we assigned risk behaviors that were significantly identified in the multivariate analysis as variables to calculate the health risk score. Assessments of health behavior as a health risk score were developed as described previously [19]. Briefly, we used the coefficients of the Cox proportional hazard model and organized the risk and protective factors with p-values <0.1 into categories. After determining the reference values for each, we computed how far each risk factor category was from the baseline category in terms of the coefficient. We then weighted them with points proportional to the β regression coefficient values, and points were rounded to the nearest integer. A health risk score was calculated for each study participant and they were grouped according to their total points and all-cause premature mortality, and hazard ratios were calculated. Three different risk groups were categorized according to their magnitude and Kaplan-Meier survival curves were drawn for the three groups. All analyses were conducted using the SAS version 9.2 (SAS Inc., Cary, NC, USA).
METHODS
- General characteristics are shown in Table 1. Age at entry, education level, smoking, and drinking status were significantly different between the live cohorts and cohorts with premature death. Table 2 shows causes of death in cohorts with ICD-10 codes. Cancer (54.0%) was the leading cause of death, followed by cardiovascular disease (9.6%) and cerebrovascular disease (7.2%).
- Of the 14 533 males who completed the baseline questionnaire survey, after excluding those with cancer, cerebrovascular disease, or myocardial infarction, a cohort of 14 205 remained for the multivariate analysis. Table 3 presents the hazard ratios (HRs) and their 95% CIs for premature mortality associated with each health behavior. In the multivariate analysis, higher age group, current smoking, current drinking, BMI ≥25, sleeping hour ≤5, education below middle school, and self-reporting of hypertension and diabetes were associated with premature mortality, while regular exercise (≥4 times per week) showed a protective effect against premature mortality. The risk increased linearly with age, with those 55 to 59 years of age having the highest risk of premature mortality with 9 points; other health behaviors varied between -1 to 5.
- After excluding subjects without information on the health behaviors selected for the health risk score calculation, each cohort participant's total health risk score was calculated. Mortality risk (%) increased as total score increased (p-trend < 0.01) (Table 4). Compared to those with 1 to 3 points, those with 22 to 25 points were at an 11.09-fold higher risk, and those with 26 to 28 points were at a 16.92-fold higher risk of premature mortality. Figure 1 shows the Kaplan-Meier curves stratified into three groups based on risk scores of 1 to 9, 10 to 19, and 20 to 28 points. The corresponding log-rank test p-value is <0.01.
RESULTS
- In this study, we examined both individual and combined impacts of health behaviors in middle-aged men in Korea using the Seoul Male Cohort Study. We found a significantly increased risk of premature mortality associated with current smoking and drinking, high BMI, fewer sleep hours, and less education. There was a strong trend towards an increase in mortality risk as the score increased and, when stratified into three groups according to points, the HR of participants with a score of 20 to 28 points indicated the highest risk of premature mortality.
- Health behaviors such as smoking, drinking, and physical inactivity are associated with both mortality and the development of chronic disease among Koreans, as determined by studies using multivariate modeling with statistical adjustments for other risk factors and confounders [20-22]. A study that evaluated smoking and mortality using the Korean Multicenter Cancer Cohort reported that smoking was significantly associated with an increased risk of mortality, especially lung cancer mortality [20]. Another study that investigated smoking-attributable mortality among Korean adults found that the smoking-related death rate was about 30.8% in male adults [21]. A case-control study that evaluated the effects of excessive drinking on mortality found significant adverse effects of alcohol dependence on both mortality and chronic health conditions [22]. Other studies have reported a protective effect of regular exercise and physical activity on both morbidity and mortality in Koreans [3,23].
- Due to complex interactions between health behaviors and the high correlation between risk factors, recent studies have focused on the combined impacts of health behaviors. The EPIC-Norfolk prospective population study reported that people with no healthy behaviors were at an increased risk of all-cause mortality, by 4.04 times [9]. The four healthy behaviors used in the EPIC-Norfolk study were current non-smoking, not physically inactive, moderate alcohol intake, and plasma vitamin C >50 mmol/L, indicating a fruit and vegetable intake of at least five servings per day. The Hale project investigated the single and combined effects of health behaviors on all-cause and cause-specific mortality in elderly European individuals, and used adherence to a Mediterranean diet, moderate alcohol use, physical activity, and nonsmoking as four healthy behaviors [10]. In our study, we not only included health behaviors, such as smoking, drinking, physical activity, and sleeping hours, but also considered BMI and education level.
- Our findings are consistent with previous findings from studies that have evaluated the combined impact of health behaviors [9-12]. The presently selected health risk behaviors overlapped with well-known poor health behaviors. However, the magnitude of the combined risk is generally higher in this study as compared with previous reports [9-12]. Previous studies did not weight different risk factors, even though there are clear differences between different risk factors in terms of the magnitude of their respective effects on mortality. In this study, we generated a scoring system to weight different health risk behaviors by considering their actual effect size on premature mortality. The group with 26 to 28 points had a 16.92-fold higher risk of premature death than the group with 1 to 3 points in our study. This suggests that the combined effects of health risk behaviors should be assessed and weighted in terms of their impact.
- This health risk score system represents an effort to make tools available to clinicians to aid in their decision-making process regarding the practice of preventative services and to assist them in motivating patients to adopt healthier behaviors. In our scoring system, non-modifiable factors such as age and education level were included. In particular, age had the highest impact on mortality. It should be noted that this system is one means of simplifying the assessment of the multi-factorial nature of mortality. Theoretical and statistical models were used to develop this scoring system, therefore applying it to the general population remains to be validated. This scoring system is one approach for making complex statistical models useful to practitioners. The scoring system used in this study has been widely used to develop scoring systems for cardiovascular diseases [24-26]. However, one limitation of using a points system rather than the Cox model is that, to achieve simplicity in use, we lose some of the information that is only captured using the entire Cox model.
- This study has several strengths. First, this is a prospective cohort study with a follow-up period of 15 years. A baseline questionnaire survey was performed at the initial recruitment and only those who were considered to be free of disease at the health screening were included. Thus, there is a clear temporal relationship between health behaviors and outcome, which leads to a clear causal relationship. In addition, there have been nearly 1000 deaths to date in the cohort, representing about 7% of all study participants. Methodological advances in considering different effect sizes when evaluating combined effects of health behaviors reflect actual phenomena more accurately than just quantifying risk factors.
- Nevertheless, there are some limitations to this study. First, the questionnaire survey was only performed once at the baseline period, even with the knowledge that some health behaviors change over time. However, by definition, the aim of this study was to identify health-related behaviors at the time of initial assessment and their association with premature mortality, and this should be differentiated from health-related behaviors over the follow-up period. Generally, it is known that lifestyle habits are characteristics of a person's way of living and reflect life-long health habits [27,28]. Second, all deaths among participants were counted as premature deaths. The life expectancy of participants ranged from 19.49 to 31.54 in 1992, and the shortest life expectancy was still longer than the follow-up period. Thus, there needs to be a longer follow-up period to ascertain all premature deaths from the study population. Moreover, we used all causes of death, even including 'Others', which accounted for 22.2% of all deaths. Third, dietary habits and laboratory findings were not included in our analysis to calculate health risk scores. In addition, when assessing alcohol intake in this study, we used current and past alcohol drinking rather the total amount of alcohol intake. To develop a more accurate health risk scoring system, further studies that incorporate dietary habits and laboratory findings are required. However, the aim of the present study was to examine the use of a simple score that could be conceptually easy to understand and used in clinical practice, rather than complex algorithms.
- In conclusion, in this prospective cohort study, smoking, drinking alcohol, physical exercise, sleep hours, education level, and BMI were associated with premature mortality. When combined, there was a strong trend towards increased mortality risk as the score increased. This finding suggests that modifiable risk factors, such as smoking, drinking, and physical activity, have considerable impacts on premature mortality. Interventions for patients at a high risk of premature mortality should stress various preventative measures that consider combined health behaviors. Further studies are required to validate the developed scoring system and to focus on not just on all causes of premature mortality, but also age-specific and cause-specific premature mortality, such as cardiovascular disease and cancer mortality.
DISCUSSION
ACKNOWLEDGEMENTS
-
The authors have no conflicts of interest with the material presented in this paper.
-
This article is available at http://jpmph.org/.
Notes
- 1. Bae JM, Lee MS, Shin MH, Kim DH, Li ZM, Ahn YO. Cigarette smoking and risk of lung cancer in Korean men: the Seoul Male Cancer Cohort Study. J Korean Med Sci 2007;22(3):508-512. 17596662ArticlePubMedPMC
- 2. Kim MK, Ko MJ, Han JT. Alcohol consumption and mortality from all-cause and cancers among 1.34 million Koreans: the results from the Korea national health insurance corporation's health examinee cohort in 2000. Cancer Causes Control 2010;21(12):2295-2302. 20941640ArticlePubMed
- 3. Kim DS, Koo HW, Kim DH, Bae JM, Shin MH, Lee MS, et al. A cohort study of physical activity and all cause mortality in middle-aged men in Seoul. Korean J Prev Med 1998;31(4):604-615. (Korean)
- 4. Doll R, Peto R, Boreham J, Sutherland I. Mortality from cancer in relation to smoking: 50 years observations on British doctors. Br J Cancer 2005;92(3):426-429. 15668706ArticlePubMedPMC
- 5. Warburton DE, Nicol CW, Bredin SS. Health benefits of physical activity: the evidence. CMAJ 2006;174(6):801-809. 16534088ArticlePubMedPMC
- 6. Van den Brandt PA. The impact of a Mediterranean diet and healthy lifestyle on premature mortality in men and women. Am J Clin Nutr 2011;94(3):913-920. 21795445ArticlePubMed
- 7. Katz DL. Life and death, knowledge and power: why knowing what matters is not what's the matter. Arch Intern Med 2009;169(15):1362-1363. 19667297ArticlePubMed
- 8. Yoo KY, Shin HR. Cancer epidemiology and prevention. Korean J Epidemiol 2003;25(1):1-15. (Korean)
- 9. Khaw KT, Wareham N, Bingham S, Welch A, Luben R, Day N. Combined impact of health behaviours and mortality in men and women: the EPIC-Norfolk prospective population study. PLoS Med 2008;5(1):e12. 18184033ArticlePubMedPMC
- 10. Knoops KT, de Groot LC, Kromhout D, Perrin AE, Moreiras-Varela O, Menotti A, et al. Mediterranean diet, lifestyle factors, and 10-year mortality in elderly European men and women: the HALE project. JAMA 2004;292(12):1433-1439. 15383513ArticlePubMed
- 11. Van Dam RM, Li T, Spiegelman D, Franco OH, Hu FB. Combined impact of lifestyle factors on mortality: prospective cohort study in US women. BMJ 2008;337: a1440. 18796495ArticlePubMedPMC
- 12. Kvaavik E, Batty GD, Ursin G, Huxley R, Gale CR. Influence of individual and combined health behaviors on total and cause-specific mortality in men and women: the United Kingdom health and lifestyle survey. Arch Intern Med 2010;170(8):711-718. 20421558ArticlePubMed
- 13. Centers for Disease Control. Premature mortality in the United States: public health issues in the use of years of potential life lost. MMWR Morb Mortal Wkly Rep 1986;35(2 Suppl):1S-11S
- 14. Shin MH, Kim DH, Bae JM, Lee HK, Lee MS, Noh JY, et al. The effect of coffee consumption on serum total cholesterol level in healthy middle-aged men. Korean J Prev Med 1994;27(2):200-216. (Korean)
- 15. Bae JM, Ahn YO. A nested case-control study on the high-normal blood pressure as a risk factor of hypertension in Korean middle-aged men. J Korean Med Sci 2002;17(3):328-336. 12068135ArticlePubMedPMC
- 16. Lee MS, Kang WC, Kim DH, Bae JM, Shin MH, Lee YJ, et al. Methodologic considerations on the cohort study of risk factors of stomach cancer: on the incompleteness of case ascertainment. Korean J Epidemiol 1997;19(2):152-160. (Korean)
- 17. WHO Expert Consultation. Appropriate body-mass index for Asian populations and its implications for policy and intervention strategies. Lancet 2004;363(9403):157-163. 14726171ArticlePubMed
- 18. Korean Statistical Information Service. Lifetable from 1970-2009. cited 2011 Dec 20. Available from: http://kosis.kr/index/index.jsp
- 19. Sullivan LM, Massaro JM, D'Agostino RB Sr. Presentation of multivariate data for clinical use: the Framingham Study risk score functions. Stat Med 2004;23(10):1631-1660. 15122742ArticlePubMed
- 20. Lee EH, Park SK, Ko KP, Cho IS, Chang SH, Shin HR, et al. Cigarette smoking and mortality in the Korean Multicenter Cancer Cohort (KMCC) study. J Prev Med Public Health 2010;43(2):151-158. (Korean). 20383048ArticlePubMedPDF
- 21. Jee SH, Lee JK, Kim IS. Smoking-attributable mortality among Korean adults: 1981-2003. Korean J Epidemiol 2006;28(1):92-99. (Korean)
- 22. Min S, Noh S, Shin J, Ahn JS, Kim TH. Alcohol dependence, mortality, and chronic health conditions in a rural population in Korea. J Korean Med Sci 2008;23(1):1-9. 18303191ArticlePubMedPMC
- 23. Park MS, Chung SY, Chang Y, Kim K. Physical activity and physical fitness as predictors of all-cause mortality in Korean men. J Korean Med Sci 2009;24(1):13-19. 19270807ArticlePubMedPMC
- 24. Rassi A Jr, Rassi A, Little WC, Xavier SS, Rassi SG, Rassi AG, et al. Development and validation of a risk score for predicting death in Chagas' heart disease. N Engl J Med 2006;355(8):799-808. 16928995ArticlePubMed
- 25. Lewis EF, Solomon SD, Jablonski KA, Rice MM, Clemenza F, Hsia J, et al. Predictors of heart failure in patients with stable coronary artery disease: a PEACE study. Circ Heart Fail 2009;2(3):209-216. 19808342ArticlePubMedPMC
- 26. Schnabel RB, Sullivan LM, Levy D, Pencina MJ, Massaro JM, D'Agostino RB Sr, et al. Development of a risk score for atrial fibrillation (Framingham Heart Study): a community-based cohort study. Lancet 2009;373(9665):739-745. 19249635ArticlePubMedPMC
- 27. Wannamethee SG, Shaper AG, Walker M. Changes in physical activity, mortality, and incidence of coronary heart disease in older men. Lancet 1998;351(9116):1603-1608. 9620713ArticlePubMed
- 28. Paffenbarger RS Jr, Hyde RT, Wing AL, Lee IM, Jung DL, Kampert JB. The association of changes in physical-activity level and other lifestyle characteristics with mortality among men. N Engl J Med 1993;328(8):538-545. 8426621ArticlePubMed
REFERENCES
Figure & Data
References
Citations

- Non-occupational physical activity and risk of cardiovascular disease, cancer and mortality outcomes: a dose–response meta-analysis of large prospective studies
Leandro Garcia, Matthew Pearce, Ali Abbas, Alexander Mok, Tessa Strain, Sara Ali, Alessio Crippa, Paddy C Dempsey, Rajna Golubic, Paul Kelly, Yvonne Laird, Eoin McNamara, Samuel Moore, Thiago Herick de Sa, Andrea D Smith, Katrien Wijndaele, James Woodcock
British Journal of Sports Medicine.2023; 57(15): 979. CrossRef - Coffee and tea consumption and mortality from all causes, cardiovascular disease and cancer: a pooled analysis of prospective studies from the Asia Cohort Consortium
Sangah Shin, Jung Eun Lee, Erikka Loftfield, Xiao-Ou Shu, Sarah Krull Abe, Md Shafiur Rahman, Eiko Saito, Md Rashedul Islam, Shoichiro Tsugane, Norie Sawada, Ichiro Tsuji, Seiki Kanemura, Yumi Sugawara, Yasutake Tomata, Atsuko Sadakane, Kotaro Ozasa, Isao
International Journal of Epidemiology.2022; 51(2): 626. CrossRef - Association between body mass index and oesophageal cancer mortality: a pooled analysis of prospective cohort studies with >800 000 individuals in the Asia Cohort Consortium
Sangjun Lee, Jieun Jang, Sarah Krull Abe, Shafiur Rahman, Eiko Saito, Rashedul Islam, Prakash C Gupta, Norie Sawada, Akiko Tamakoshi, Xiao-Ou Shu, Woon-Puay Koh, Atsuko Sadakane, Ichiro Tsuji, Jeongseon Kim, Isao Oze, Chisato Nagata, San-Lin You, Myung-He
International Journal of Epidemiology.2022; 51(4): 1190. CrossRef - Burden of Cancer Due to Cigarette Smoking and Alcohol Consumption in Korea
Yoon-Sun Jung, Seok-Jun Yoon
International Journal of Environmental Research and Public Health.2022; 19(6): 3493. CrossRef - First Report on the Co-Occurrence and Clustering Profiles of Cardiovascular Lifestyle Risk Factors among Adults in Burkina Faso
Kadari Cissé, Sékou Samadoulougou, Yves Coppieters, Bruno Bonnechère, Patrice Zabsonré, Fati Kirakoya-Samadoulougou, Seni Kouanda
International Journal of Environmental Research and Public Health.2022; 19(14): 8225. CrossRef - Associations Between Self-Reported Sleep Duration and Mortality in Employed Individuals: Systematic Review and Meta-Analysis
Paula R. Pienaar, Tracy L. Kolbe-Alexander, Willem van Mechelen, Cécile R. L. Boot, Laura C. Roden, Estelle V. Lambert, Dale E. Rae
American Journal of Health Promotion.2021; 35(6): 853. CrossRef - Public health nurses’ workforce factors and population health outcomes in the United States
Seok Hyun Gwon, Young Ik Cho, Soonhwa Paek, Weiming Ke
Public Health Nursing.2020; 37(6): 829. CrossRef - Patterns of change in cardiovascular risks of Korean male workers: a 10-year cohort analysis using the National Health Insurance Service–National Sample Cohort (NHIS-NSC) 2.0 database
Hosihn Ryu, Jiyeon Jung, Jihyun Moon
BMJ Open.2020; 10(11): e038446. CrossRef - Sleep duration and mortality in Korean adults: a population-based prospective cohort study
Sohyeon Kwon, Hyeyoung Lee, Jong-Tae Lee, Min-Jeong Shin, Sangbum Choi, Hannah Oh
BMC Public Health.2020;[Epub] CrossRef - Sleep duration and risk of all-cause mortality: a systematic review and meta-analysis
H. A. García-Perdomo, J. Zapata-Copete, C. A. Rojas-Cerón
Epidemiology and Psychiatric Sciences.2019; 28(5): 578. CrossRef - Time trends in healthy lifestyle among adults in Germany: Results from three national health interview and examination surveys between 1990 and 2011
Jonas D. Finger, Markus A. Busch, Christin Heidemann, Cornelia Lange, Gert B. M. Mensink, Anja Schienkiewitz, David Meyre
PLOS ONE.2019; 14(9): e0222218. CrossRef - Simple sleep questions can predict 12-year mortality in a rural population
Christina Darviri, Artemios Artemiadis, Xanthi Tigani, Panagiota Darvyri, Charalambos Gnardellis
Sleep and Biological Rhythms.2018; 16(2): 253. CrossRef - Self‐Reported Sleep Duration and Quality and Cardiovascular Disease and Mortality: A Dose‐Response Meta‐Analysis
Chun Shing Kwok, Evangelos Kontopantelis, George Kuligowski, Matthew Gray, Alan Muhyaldeen, Christopher P. Gale, George M. Peat, Jacqueline Cleator, Carolyn Chew‐Graham, Yoon Kong Loke, Mamas Andreas Mamas
Journal of the American Heart Association.2018;[Epub] CrossRef - Sleep duration and risk of all-cause mortality: A flexible, non-linear, meta-regression of 40 prospective cohort studies
Tong-Zu Liu, Chang Xu, Matteo Rota, Hui Cai, Chao Zhang, Ming-Jun Shi, Rui-Xia Yuan, Hong Weng, Xiang-Yu Meng, Joey S.W. Kwong, Xin Sun
Sleep Medicine Reviews.2017; 32: 28. CrossRef - Cohort Profile:Ten to Men(the Australian Longitudinal Study on Male Health)
Jane Pirkis, Dianne Currier, John Carlin, Louisa Degenhardt, Shyamali C. Dharmage, Billie Giles-Corti, Ian R. Gordon, Lyle C. Gurrin, Jane S. Hocking, Anne Kavanagh, Louise Keogh, Rachel Koelmeyer, Anthony D. LaMontagne, George Patton, Lena Sanci, Matthew
International Journal of Epidemiology.2016; : dyw055. CrossRef - The Australian longitudinal study on male health-methods
Dianne Currier, Jane Pirkis, John Carlin, Louisa Degenhardt, Shyamali C. Dharmage, Billie Giles-Corti, Ian Gordon, Lyle Gurrin, Jane Hocking, Anne Kavanagh, Louise A. Keogh, Rachel Koelmeyer, Anthony D. LaMontagne, Marisa Schlichthorst, George Patton, Len
BMC Public Health.2016;[Epub] CrossRef - The relationship between mild alcohol consumption and mortality in Koreans: a systematic review and meta-analysis
Ji-Eun Park, Tae-young Choi, Yeonhee Ryu, Sung-Il Cho
BMC Public Health.2015;[Epub] CrossRef - Adverse Lifestyle Leads to an Annual Excess of 2 Million Deaths in China
G. Neil Thomas, Man Ping Wang, Sai Yin Ho, Kwok Hang Mak, Kar Keung Cheng, Tai Hing Lam, Hamid Reza Baradaran
PLoS ONE.2014; 9(2): e89650. CrossRef - Cardiovascular Health Metrics and All-cause and Cardiovascular Disease Mortality Among Middle-aged Men in Korea: The Seoul Male Cohort Study
Ji Young Kim, Young-Jin Ko, Chul Woo Rhee, Byung-Joo Park, Dong-Hyun Kim, Jong-Myon Bae, Myung-Hee Shin, Moo-Song Lee, Zhong Min Li, Yoon-Ok Ahn
Journal of Preventive Medicine and Public Health.2013; 46(6): 319. CrossRef - The combined effects of healthy lifestyle behaviors on all cause mortality: A systematic review and meta-analysis
Martin Loef, Harald Walach
Preventive Medicine.2012; 55(3): 163. CrossRef
 KSPM
KSPM

 PubReader
PubReader ePub Link
ePub Link Cite
Cite


