Congenital Malformations in Infants of Mothers Undergoing Assisted Reproductive Technologies: A Systematic Review and Meta-analysis Study
Article information
Abstract
Objectives
This meta-analysis aimed to evaluate congenital malformations in infants conceived by assisted reproductive techniques (ART), compared with infants conceived spontaneously.
Methods
In this study, available resources searched to find relevant articles included PubMed, ScienceDirect, Scopus, Google Scholar, Cochrane, ProQuest, Iranmedex, Magiran, and Scientific Information Database. After extracting the necessary information from evaluated articles, meta-analysis on the articles’ data was performed using Stata version 11.2.
Results
In this study, from a total of 339 articles, extracted from the initial investigation, ultimately 30 articles were selected for meta-analysis that assessed the use of ART on the risk of congenital abnormalities and some birth complications on 5 470 181 infants (315 402 cases and 5 154 779 controls). The odds ratio (95% confidence interval [CI]) for low birth weight was 1.89 (95% CI, 1.36 to 2.62), preterm labor 1.79 (95% CI, 1.21 to 2.63), cardiac abnormalities 1.43 (95% CI, 1.27 to 1.62), central nervous system abnormalities 1.36 (95% CI, 1.10 to 1.70), urogenital system abnormalities 1.58 (95% CI, 1.28 to 1.94), musculoskeletal disorders 1.35 (95% CI, 1.12 to 1.64), and chromosomal abnormalities in infants conceived by ART was 1.14 (95% CI, 0.90 to 1.44), which were all statistically significant, except chromosomal abnormalities.
Conclusions
The risk of congenital abnormalities and some birth complications were significantly higher in ART than normal conception, while chromosomal abnormalities were not; therefore, the application of ART should be selected individually for patients by detailed assessment to reduce such risks in the population.
INTRODUCTION
Assisted reproductive technologies (ART) include 1% of births in the US and 4.3% of births in European countries and Australia [1]. Scientific and medical advances have increased the pregnancy rates and births following ART can be expected to rise. Any method or medication to achieve pregnancy is accepted as a broad definition of the concept of ART, which includes ovulation induction, intrauterine insemination, in vitro fertilization (IVF), and intracytoplasmic sperm injection (ICSI) [2]. Application of these methods has solved the infertility problem of human and had multiple health benefits for millions of couples suffering from fertility problems [3]. During the past 36 years, ART has reformed from a miracle to a standard and common part of medical practice. More than 200 000 infants are annually born worldwide by this technology [2]. It is estimated that over 5 million children worldwide have been born after ART procedures [1]. There are worldwide 72.4 million infertile women and 21-22% of women in our country experience primary infertility in their marital life. Worldwide, about 40 million couples benefit from reproductive medicine [4,5]. All these figures indicate that since the birth of Louise Brown, the first baby born after artificial insemination in 1978 in the UK, ART have advanced quickly that have attracted more and more researcher’s attention towards the risks and complications of this method [6]. Developed and advanced use of this method has increased the rate of infants born by this method and have pursued researchers to follow these children’s health status [7].
After 30 years of using ART, there are evidence of increased adverse perinatal outcomes such as premature birth (PTB), low birth weight (LBW) and small for gestational age infants, compared with children conceived spontaneously [8]. Studies show that ART can increase the incidence of congenital malformations at 25-40% [9] and these children are at risk of a range of disabilities [10].
Various artificial methods, performed during ART treatment, imply the concern that infants conceived through these methods are at higher risk than infants conceived spontaneously. In such methods, firstly, many drugs are prescribed to stimulate ovulation, oocyte retrieval, and embryos cultured, frozen and melt in vitro, and high doses of progesterone for luteal phase support, which may all damage gametes or embryos. In addition, ICSI method, in which an egg is fertilized by injecting sperm directly into ooplasm, is considered more invasive than IVF. It also significantly increases the risk of multiple pregnancies by transferring more than one embryo, which leads to risk of complications such as PTBs and LBW [3].
The results of some studies indicate that infants conceived through ART are at higher risk of congenital abnormalities than normal pregnancies, but some other studies have not observed such difference or have even reported less risk, especially in multiple pregnancies [6].
Regarding the conflicting results and as far as some complications can cause malformations that increase in infants conceived through this method, such as preterm labor and LBW, thus, this meta-analysis study aimed to assess the complications and the risk of some congenital malformations including cardiovascular, central nervous system, musculoskeletal, urogenital and chromosomal abnormalities in newborns conceived following ART compared to infants conceived spontaneously.
METHODS
In this study, available resources searched to find relevant articles included PubMed, ScienceDirect, Scopus, Google Scholar, Cochrane, ProQuest, Iranmedex, Magiran, and Scientific Information Database (SID) databases, published from 2005 to 2015. We retrieved 201 citations in PubMed, 38 citations in Scopus, 55 citations in EMBASE, 10 citations in Google Scholar, 15 citations in Cochrane, 16 citations in ProQuest, 4 citations in Iranmedex, 0 citation in Magiran and 0 citation in SID.
In order to avoid losing resources, congress performances, theses, books and other domestic and foreign valid websites were manually searched. List of references used in all articles and related reports found by the electronic search were evaluated manually to include other possible sources in the study.
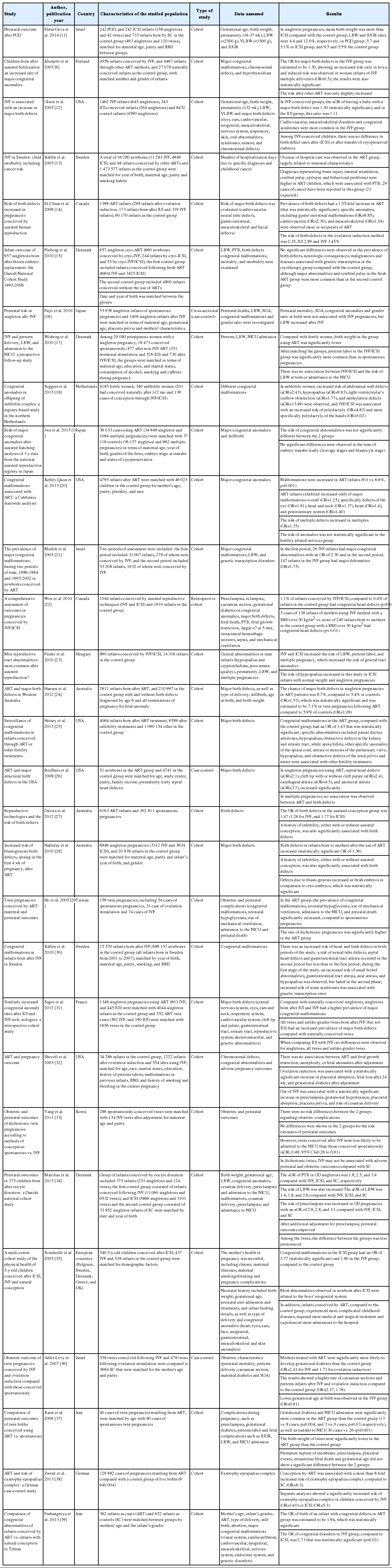
The searched keywords included (birth defect or congenital malformation or congenital abnormalities) and (ART or IVF or ICSI). After preparation of the initial list, two colleagues examined titles and abstracts independently and identified relevant articles. Then, they registered closely-related or possibly-related studies and selected related studies by examining the full text of articles. At the end, among the articles selected based on critical evaluation, articles that met the inclusion criteria were finally selected (Table 1).
To include the study objectives, all articles with the following inclusion criteria were extracted: Access to full-text articles in English; Cohort or case-control studies; The study population including infants conceived through ART vs. control group over a period of time.
Data Extraction and Quality Evaluation
All identified papers were critically appraised independently by two reviewers (SC and YM). Any disagreement was assessed by both and if a consensus was not reached, a third author (HH) evaluated the study. Two independent matched reviewers (PM and YM) extracted data according to a uniform Excel sheet. Disagreements between reviewers were resolved by consensus. Appraisal was guided by checklist assessing clarity of the aims and research questions. STROBE (Strengthening the Reporting of Observational Studies in Epidemiology) checklist score was used as a standard checklist for reporting the results of the included studies. Then, the closely-related or possibly-related studies were listed and selected by examining the full text of eligible articles. At the end, among selected articles, based on critical evaluation, articles that met the inclusion criteria were ultimately selected (Table 1). Some of the information, including odds ratio (OR) in some studies and confidence interval (CI), p-value, number of samples extracted from the articles, the standard error, variance and the logarithm of the variance and weight of articles were calculated using available data in the literature.
Data Analysis
After extracting the necessary information from evaluated articles, meta-analysis on the articles’ data was performed using Stata version 11.2 (StataCorp, College Station, TX, USA). Metan order was used to analyze the data, and Q-test and I2 were used to measure heterogeneity of studies and Begg’s funnel plot to assess publication bias.
RESULTS
In this study, from a total of 339 articles extracted from the initial investigation, ultimately 30 articles were selected for meta-analysis tests that assessed the use of ART on the risk of congenital abnormalities and some birth complications on 5 470 181 infants (315 402 cases and 5 154 779 controls). All studies were evaluated by two independent researchers and, in case of disagreement, a third arbitrator examined to rule out the study.
Supplemental Tables 1 and 2 show the results of the meta-analysis, the OR for congenital malformations and birth complications among infants conceived through ART. The estimated OR for congenital abnormalities in infants conceived by ART was 1.53 (95% CI, 1.37 to 1.70), which was statistically significant. This means that infants conceived through ART are at 53% increased risk of congenital abnormalities than other infants. The results partly reflect the heterogeneity of the studies (χ2=214.43; p<0.001; I2=89.7%), but since the CI of test (Egger’s test) included zero, no significant bias occurred in the publication of the results. The estimated OR for LBW in infants conceived by ART was 1.89 (95% CI. 1.36 to 2.62), which was statistically significant. This means that infants conceived through ART are at 89% increased risk of LBW than other infants. The results partly reflect the heterogeneity of the studies (χ2=2174.05; p<0.001; I2=99.3%), but since the CI of test (Egger’s test) included zero, no significant bias occurred in the publication of the results.
The estimated OR for preterm labor in infants conceived by ART was 1.79 (95% CI, 1.21 to 2.63), which was statistically significant. This means that infants conceived through ART are at 79% increased risk of preterm labor than other infants. The results partly reflect the heterogeneity of the studies (χ2= 3089.90; p<0.001; I2=99.6%), but since the CI of test (Egger’s test) included zero, no significant bias occurred in the publication of the results (Table 2).

Results of the meta-analysis of the odds of preterm labor and cardiovascular abnormalities in ART infants
The estimated OR for cardiac malformations in infants conceived by ART was 1.43 (95% CI, 1.27 to 1.27), which was statistically significant. This means that infants conceived through ART are at 43% increased risk of cardiac malformations than other infants. The results partly reflect the heterogeneity of the studies (χ2=31.12; p=0.003; I2=58.2%), but since the CI of test (Egger’s test) included zero, no significant bias occurred in the publication of the results (Table 2).
The estimated OR for central nervous system malformations in infants conceived by ART was 1.36 (95% CI, 1.10 to 1.70), which was statistically significant. This means that infants conceived through ART are at 36% increased risk of central nervous system malformations than other infants. The results partly reflect the heterogeneity of the studies (χ2=25.67; p=0.002; I2=64.9%), but since the CI of test (Egger’s test) included zero, no significant bias occurred in the publication of the results (Supplemental Table 2).
The estimated OR for urogenital malformations in infants conceived though ART was 1.58 (95% CI, 1.28 to 1.94), which was statistically significant. This means that infants conceived though ART are at 58% increased risk of urogenital malformations than other infants. The results partly reflect the heterogeneity of the studies (χ2=65.26; p<0.001; I2=81.6%), but since the CI of test (Egger’s test) included zero, no significant bias occurred in the publication of the results (Supplemental Table 2).
The estimated OR for musculoskeletal malformations in infants conceived by ART was 1.35 (95% CI, 1.12 to 1.64), which was statistically significant. This means that infants conceived through ART are at 35% increased risk of musculoskeletal malformations at 35%. The results partly reflect the heterogeneity of the studies (χ2=34.93; p<0.001; I2=74.06%), but since the CI of test (Egger’s test) included zero, no significant bias occurred in the publication of the results (Table 3).

Results of the meta-analysis of the odds of musculoskeletal abnormalities and chromosomal abnormalities in ART infants
The estimated OR for chromosomal disorders in infants conceived by ART was 1.14 (95% CI, 0.90 to 1.44), which was not statistically significant. This means that infants conceived through ART are at 14% increased risk of chromosomal disorders than other infants that was not statistically significant. The results partly reflect the heterogeneity of the studies (χ2=27.93; p=0.002; I2=64.2%), but since the CI of test (Egger’s test) included zero, no significant bias occurred in the publication of the results (Table 3).
DISCUSSION
Systematic review and meta-analysis of results of studies indicated that the risk of congenital malformations in infants conceived by ART increases, compared with infants of spontaneous conception (SC; OR, 1.53; 95 CI, 1.37 to 1.70) that was statistically significant; meaning that infants conceived by ART are at 53% greater risk for congenital malformations. The results of the study by Shevell and colleagues [32] showed that abnormalities were more in IVF group than SC. Simpson [1] suggested that the use of ART are associated with a relative increase in birth defects (OR, 1.30). The meta- analysis by Hansen and Bower [40] on systematic reviews and meta-analysis studies on ART and birth defects showed that the results of six studies indicated an increase of 30-70% (OR, 1.31 to 1.70) in birth defects in the ART group. In the meta-analysis study by Pandey and colleagues [41], the OR of congenital malformations in ART infants was estimated 1.67 (95% CI, 1.33 to 2.09). The results of the study by Jie et al. [42] indicated no significant differences between the two groups of ART and SCs regarding the prevalence of birth defects (p=0.07). In the meta-analysis by Hansen et al. [43] on 45 studies, the OR of congenital malformations in infants conceived through ART was 1.32 (95% CI, 1.24 to 1.42) and in ART twin infants was 1.11 (95% CI, 0.98 to 1.26), which was not statistically significant.
In the present study, the results significantly showed that infants conceived by ART are 89% more born with low weight (OR, 1.89; 95% CI, 1.36 to 2.62). The results by Jamshidi et al. [44] suggested that 1% of singleton SCs were LBW, compared with 19% in singleton IVF group, with a statistically significant OR of 2.5; while, the research by Hajishafiha and colleagues [45] showed that the growth parameters and fetal development including birth weight was not statistically different between two groups of users of ART methods and SC. In the research by Yasaei and Ataei [46] birth weight and gestational age in three groups of spontaneous twin pregnancies, after IVF, and ovulation induction had no significant differences. The OR estimated in the meta-analysis of results by Helmerhorst et al. [47], Jackson et al. [48], McDonald et al. [49], and Pandey et al. [41] have reported LBW in ART group, compared to spontaneous pregnancies, OR, 1.7; 95% CI, 1.5 to 1.9; OR, 1.8; 95% CI, 1.4 to 2.2; OR, 1.6; 95% CI, 1.3 to 2.0; and OR, 1.67 95% CI, 1.6 to 1.8, respectively.
The results of the current meta-analysis on conception following ART indicated that these infants (OR, 1.79; 95% CI, 1.21 to 2.63), compared with normal pregnancies, have 79% more preterm labor that was statistically significant. Barat et al. [37] concluded in their study that the mean age in the group receiving ART were lower, compared with SC, but was not statistically significant.
Regarding the results of the meta-analysis on the likelihood of preterm labor in ART, compared with spontaneous pregnancies, Helmerhorst et al. [47] estimated the 2.0 (95% CI, 1.8 to 2.3); Jackson et al. [48] 2.0 (95% CI, 1.7 to 2.2); McGovern et al. [50] 2.0 (95% CI, 1.8 to 2.2); McDonald et al. [49] 1.8 (95% CI, 1.5 to 2.2); and Pandey et al. [41] 1.5 (95% CI, 1.5 to 1.6); these results were all significant and were almost similar to the results of the current meta-analysis.
Regarding the risk of major malformations (cardiovascular, central nervous system, musculoskeletal, urogenital and chromosomal abnormalities) in infants after ART, compared with SCs, the meta-analysis of the results indicated that infants conceived by ART were 43% more susceptible to cardiovascular abnormalities 1.43 (95% CI, 1.30 to 1.60) that was statistically significant. Among 14 studies, the OR was not only higher than one, but also statistically significant. In the meta-analysis by Wen et al. [51], the OR of births resulting from ART, compared with SC, was 1.64 (95% CI, 1.30 to 2.17) that was statistically significant.
The results of the meta-analysis of the results of the central nervous system disorders suggested that infants conceived by ART develop this complication 36% more than infants conceived spontaneously OR=1.36 (95% CI, 1.10 to 1.70). Among 10 studies included in the current meta-analysis, only one case estimated the OR of birth of an infant with central nervous system less than one and was in four studies not only higher than one, but also statistically significant. In the meta-analysis by Wen et al. [51] the likelihood of birth of an infant with central nervous system abnormalities in ART users, compared with SC, was estimated at 2.0 (95% CI, 1.3 to 3.2) that was statistically significant.
Regarding urogenital abnormalities, the results indicated that the probability of ART infants born with these abnormalities, compared with SCs, was 58% (OR, 1.58; 95% CI, 1.28 to 1.94), more statistically significant. From 13 studies included in the meta-analysis, only one cases [19] declared an OR of less than one regarding the probability of urogenital abnormalities in ART infants and 4 studies reported higher OR that were statistically significant. A meta-analysis conducted by Wen and colleagues [51] also reported the chance of having a baby with urogenital malformations in ART group OR=1.6 (95% CI, 1.3 to 2.1) that was statistically significant and is close to the OR estimated in the present study.
In the present meta-analysis, the risk of musculoskeletal disorders in infants receiving assisted reproductive therapy was 35% (OR, 1.35; 95% CI, 1.12 to 1.64) higher than infants of SC. From eleven articles included in the meta-analysis, 7 articles reported a statistically significant OR of higher than one regarding the risk of musculoskeletal disorders in ART infants. A meta-analysis by Wen et al. [51] also reported OR of 1.48 (95% CI, 1.09 to 2.03) in this regard.
The results of the risk of chromosomal abnormalities in infants conceived by ART showed that these infants are born with 14% increased risk of chromosomal abnormalities than infants with SC (OR,1.14; 95% CI, 0.90 to 1.44), which was not statistically significant. Among eleven studies that were evaluated in the current meta-analysis, 4 studies reported an OR of less than one and only one that was statistically significant (The study by Hansen et al. [24] that estimated the possibility of having a baby with chromosomal abnormalities in infants using ART a little more than 2, compared to SCs).
The results of the current meta-analysis also indicated a remarkable discrepancy among studies that can be due to the method of assessing infants in case and control groups, as well as matching some confounding variables including mother’s age, the reason and duration of infertility, previous treatments, exposure to some environmental factors, high-risk behaviors (smoking and alcohol), and variety of ART procedures. Some researchers have concluded that the increased risk associated with the use of ART should be sought more in couple’s problems and the reason of infertility than infertility treatment.
European Society for Human Reproduction and Embryology reported on the status of patients after treatment that newborns after the use of ART methods such as IVF or ICSI are born with 40-50% more birth defects [52]. Similarly, an increased risk is reported in infertile couples conceiving spontaneously or with intervention after a long period of infertility. The main reason of this increased risk can be the genetic characteristics and special conditions occurring in couples, rather than the received treatment; it is thus suggested that future studies select the control group from infertile couples who have conceived spontaneously.
One of the most important individual effects on children’s health following increased ART treatments is the chance of multiple pregnancies occurring following transferring more than one embryo. Total risk of multiple pregnancies demonstrably increases in women using ART. Notably, most of these pregnancies are dizygotic and as far as the adverse outcomes of monozygotic pregnancies are higher, this indicates the decreased possibility of congenital malformations in multiple pregnancies following ART, compared to SCs.
CONCLUSION
It is suggested that the future meta-analysis be conducted on more detailed factors, such as comparing ART with the possibility of birth of an abnormal infant or comparing the abnormalities in singleton pregnancies with multiple pregnancies or assess the infants’ gender, in order to be able to select the safest treatment options for minimizing the risk of birth defects.
Notes
CONFLICT OF INTEREST
The authors have no conflicts of interest associated with the material presented in this paper.
SUPPLEMENTAL MATERIAL
The results of meta-analysis of the odds of congenital malformations and LBW in ART infants
The results of meta-analysis of the odds of CNS and urogenital abnormalities in ART infants