The Role of Pharmacists’ Interventions in Increasing Medication Adherence of Patients With Epilepsy: A Scoping Review
Article information
Abstract
Objectives:
Epilepsy is a chronic disease that requires long-term treatment and intervention from health workers. Medication adherence is a factor that influences the success of therapy for patients with epilepsy. Therefore, this study aimed to analyze the role of pharmacists in improving the clinical outcomes of epilepsy patients, focusing on medication adherence.
Methods:
A scoping literature search was conducted through the ScienceDirect, PubMed, and Google Scholar databases. The literature search included all original articles published in English until August 2023 for which the full text was available. This scoping review was carried out by a team consisting of pharmacists and neurologists following the Preferred Reporting Items for Systematic reviews and Meta-Analyses (PRISMA) Extension for Scoping Reviews and the Joanna Briggs Institute guidelines, including 5 steps: identifying research questions, finding relevant articles, selecting articles, presenting data, and compiling the results.
Results:
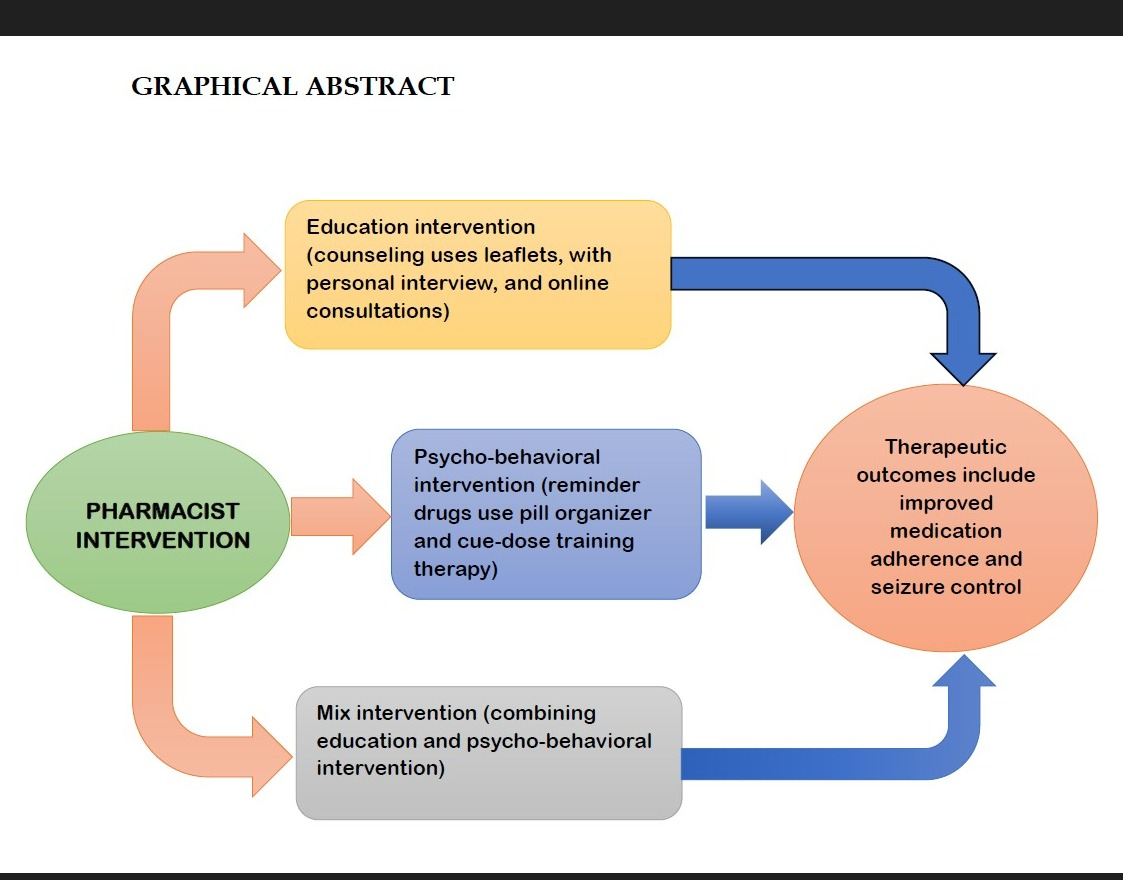
The literature search yielded 10 studies that discussed pharmacist interventions for patients with epilepsy. Five articles described educational interventions involving drug-related counseling with pharmacists. Two articles focused on similar pharmacist interventions through patient education, both verbal and written. Three articles discussed an epilepsy review service, a multidisciplinary intervention program involving pharmacists and other health workers, and a mixed intervention combining education and training with therapy-based behavioral interventions.
Conclusions:
Pharmacist interventions have been shown to be effective in improving medication adherence in patients with epilepsy. Furthermore, these interventions play a crucial role in improving other therapeutic outcomes, including patients’ knowledge of self-management, perceptions of illness, the efficacy of antiepileptic drugs in controlling seizures, and overall quality of life.
INTRODUCTION
Epilepsy is a neurological disorder characterized by the occurrence of unprovoked seizures [1]. These seizures are recurrent and result from excessive and abnormal neuronal activity in the brain, which can be caused by various factors including head trauma, stroke, or metabolic disorders [2]. According to data from the World Health Organization, it is estimated that 50 million people worldwide have epilepsy, and 70% of them could be seizure-free with proper diagnosis and treatment [3]. However, the prevalence of treatment failure is still significant, as demonstrated by the results of the Standard and New Antiepileptic Drugs trial, which reported a 29% rate of antiepileptic medication failure among patients with generalized tonic-clonic seizures [4]. Additionally, about 63% of individuals receiving epilepsy treatment show favorable seizure control in response to the prescribed therapy, while 37% experience treatment failure with poor seizure control [5]. To date, poor drug adherence remains a major cause of uncontrolled therapy in patients with epilepsy. Adherence to medication involves patient behavior in taking medication according to the prescriber’s (doctor’s) instructions [6,7]. Non-adherence to medication regimens is a potential risk for the recurrence of epilepsy and is closely linked to a higher incidence of hospitalization and increased financial burdens [8-10].
Epilepsy treatment is complex and may require multiple antiepileptic drugs, special diets, and neurostimulation [11]. Additionally, the use of antiepileptic drugs often leads to side effects and drug-drug interactions [12,13], which can result in poor patient adherence, especially among those with limited knowledge about the disease and its treatment [14]. Given these challenges, the role of pharmacists is crucial in providing education and counseling [15]. Pharmacists have demonstrated their ability to enhance medication adherence among epilepsy patients [16]. According to a systematic review by Reis et al. [17], pharmacists can positively impact epilepsy patients by increasing adherence to antiepileptic drugs, enhancing knowledge about epilepsy, and improving patients’ quality of life. One strategy of the American Epilepsy Society for managing epilepsy is to integrate pharmacists who can collaborate with other health workers to improve access to health services [18]. However, there is limited information on how pharmacists specifically contribute to increasing patients’ adherence to medication. Therefore, this literature review aims to examine the contribution of pharmacists to improving the clinical outcomes of epilepsy patients, focusing particularly on medication adherence.
METHODS
This scoping review was conducted by a team of pharmacists and neurologists in accordance with the Joanna Briggs Institute (JBI) guidelines [19] and the Preferred Reporting Items for Systematic reviews and Meta-Analyses (PRISMA) Extension for Scoping Reviews [20]. The framework for the scoping review, based on the JBI guidelines, comprises 5 stages: identifying research questions, locating relevant articles, selecting articles, presenting data, and summarizing the findings [19]. The study selection process adhered to a flowchart adapted from the PRISMA statement [20].
Identify Research Questions
The research question was as follows: how can pharmacists contribute to improving medication adherence in epilepsy patients?
Find Relevant Research
We conducted a scoping literature search using the databases ScienceDirect, PubMed, and Google Scholar. The search employed a Boolean combination of terms: (“pharmacist” or “pharmacy”) AND (“intervention”) AND (“epilepsy” or “epileptic”) AND (“adherence” or “compliance”). This search included all original articles published in English up to August 23, 2023, with full texts available. Four authors—IE, ZI, NMY, and IS—implemented a two-step procedure to select relevant articles. Initially, after eliminating duplicates, each author independently reviewed the titles and abstracts of articles that discussed interventions conducted by pharmacists for epilepsy patients, without restricting the type of intervention or study.
Research Article Selection
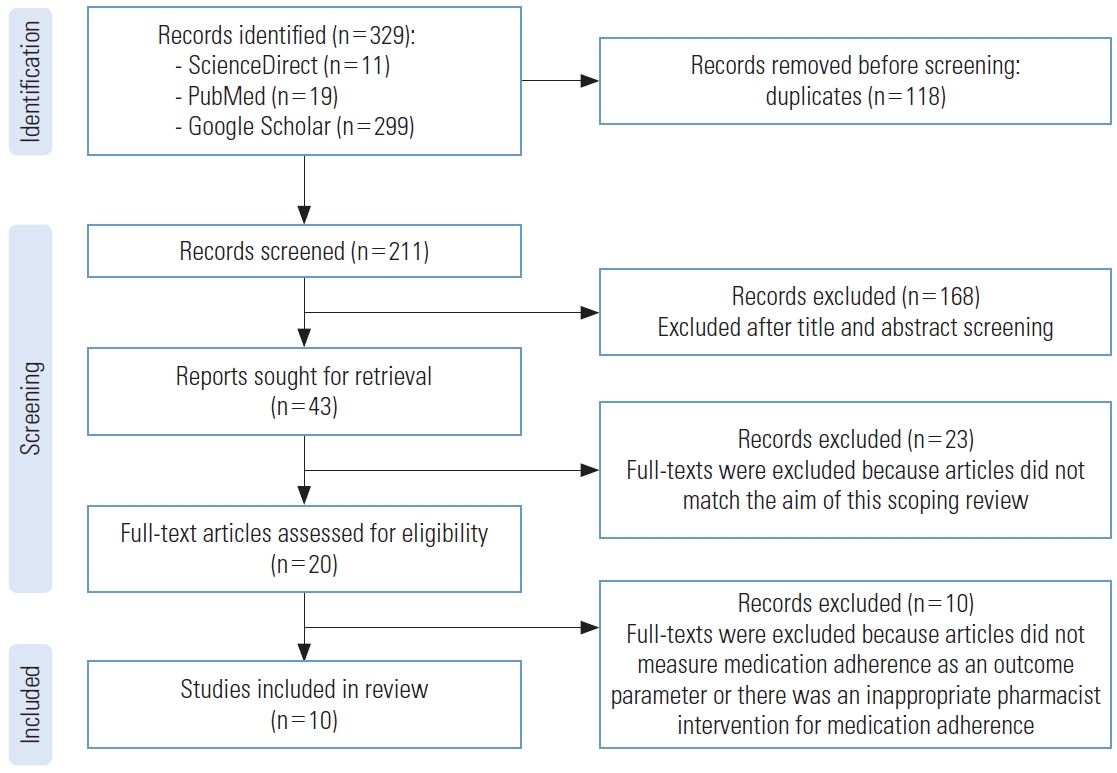
The next step was to read full-text articles that meet the inclusion criteria: (1) interventions conducted by pharmacists or in collaboration with other multidisciplinary health practitioners, (2) studies published in English, (3) no restrictions on the types of interventions provided in the full-text articles, (4) the therapeutic parameters observed included adherence, with or without secondary outcomes such as knowledge, seizure control, or quality of life (Figure 1).
Data Presentation
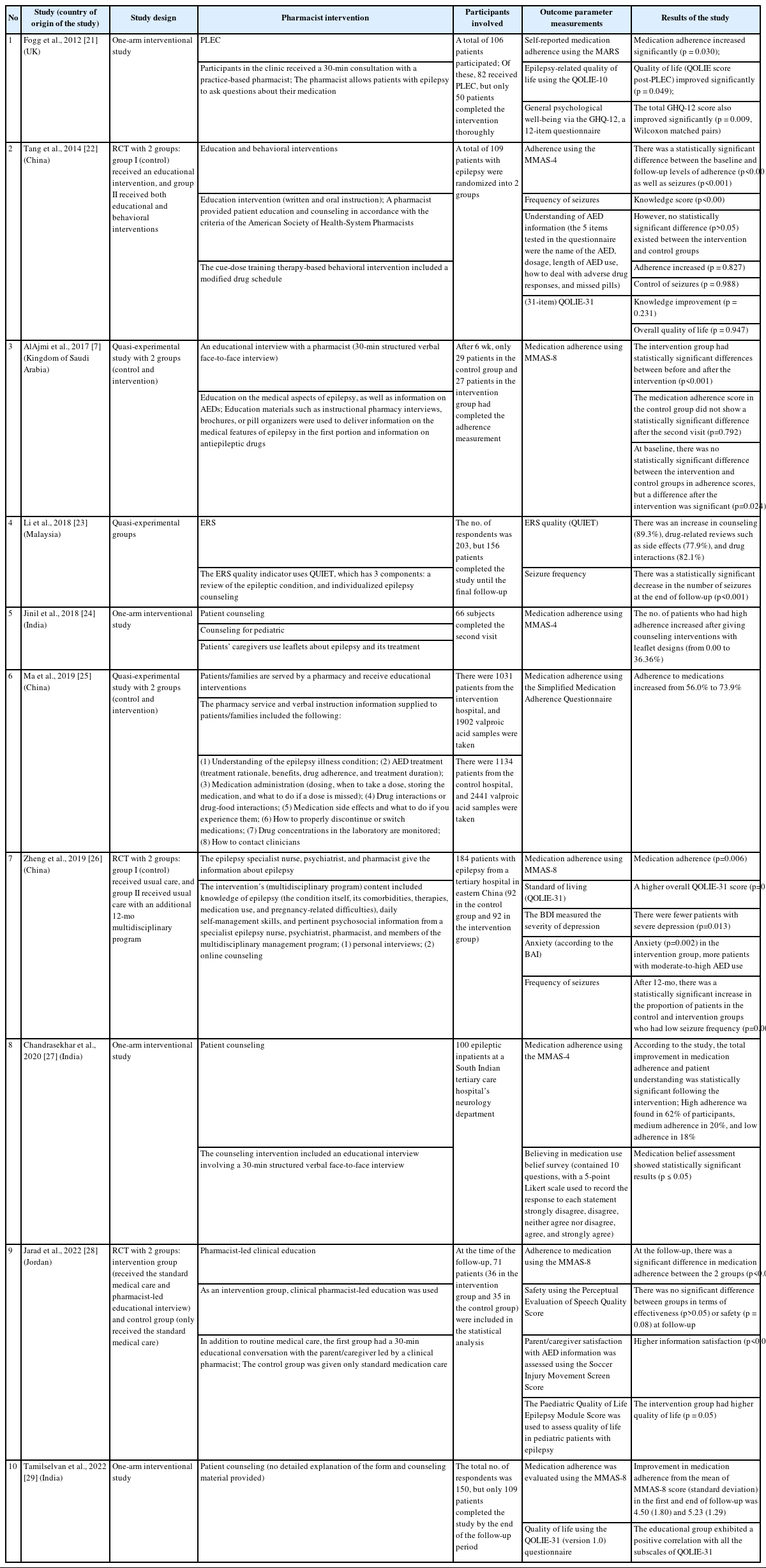
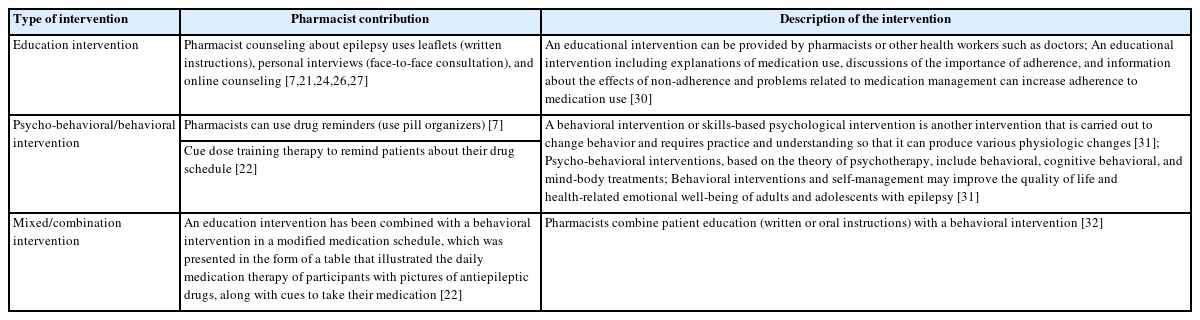
Four authors (IE, ZI, NMY, IS) were responsible for data extraction and presentation from the included studies. The tables record information such as authors, publication year, country, study design, pharmacist interventions, participants involved, outcome parameters, and study results. The data are presented through a qualitative analysis based on the existing data in each article (Table 1) [7,21-29]. Additional details about the type and description of interventions can be found in Table 2 [7,21,22,24,26,27,30-32].
Results Compilation
A series of discussions among all reviewers was conducted to refine the best approach for reviewing, summarizing, and presenting the literature findings in a consistent format. The results are organized and summarized based on their relevance to the overall research question.
Ethics Statement
As this was a scoping review, data extraction was conducted solely from published articles. Therefore, no institutional review board approval was needed.
RESULTS
A comprehensive search of the ScienceDirect, PubMed, and Google Scholar databases yielded a total of 329 entries identified as potentially relevant for the study. After screening to remove duplicates and examining the abstracts of articles used in this scoping review, 43 articles were obtained. Upon reviewing the full-text, we excluded 33 articles due to objectives that did not match and because they did not measure medication adherence as an outcome parameter. The adherence measurements used in the reviewed articles included not only questionnaires but also blood drug levels (Figure 1).
This scoping review examines all publications that involve interventions by pharmacists or pharmacy students in treating patients with epilepsy. The contributions of pharmacists identified in the studies include providing counseling (verbal, written, and online consultations), as well as setting schedules and reminders for medication adherence [7,22,25,27-29]. Additionally, pharmacists may distribute informational leaflets to patients as part of their clinical practice [24]. Educational interventions through counseling are often paired with strategies to improve adherence to drug regimens, such as modifying drug schedules to simplify medication intake [22]. Pharmacist interventions also encompass education through personal consultations, which cover understanding the disease (patient’s condition), drug use (adherence, benefits, administration methods, preparation, drug interactions, procedures for reporting side effects, seizures, and how to contact a clinician if issues arise during treatment) [23,25]. As health professionals, pharmacists collaborate with other healthcare providers in multidisciplinary programs to offer insights into epilepsy medications and therapies for comorbid conditions (Table 1) [26]. Moreover, collaboration between pharmacists and other multidisciplinary professionals is not limited to healthcare workers but can also include educators. Research by Yilmazel [33] indicates that there is generally low awareness of epilepsy, negative attitudes towards the condition, and limited health literacy among teachers and students. This highlights an opportunity for pharmacists to partner with teachers to enhance epilepsy awareness through activities such as workshops, panels, and health education training on epilepsy.
DISCUSSION
Epilepsy is a chronic condition that requires long-term treatment. The administration of antiepileptic drugs typically starts with a monotherapy at the lowest possible dose, which may be increased to achieve effective levels while minimizing side effects. If seizures continue, a combination of antiepileptic drugs may be required [34]. In this context, pharmacists play a crucial role by reviewing patient medications, conducting drug reconciliations, analyzing adverse events, and implementing interventions to enhance treatment outcomes [35]. According to ten reviewed studies, pharmacist interventions are designed to improve drug adherence through either direct or face-to-face counseling, or via digital services [26]. Direct counseling involves providing patients with detailed information about epilepsy symptoms, seizure triggers, antiepileptic drugs, medication adherence, and the effectiveness of these drugs in controlling seizures [7,21,24,27,29]. Additionally, printed leaflets containing information about epilepsy treatment can be distributed to the patient’s caregiver [24]. Moreover, Tang et al. [22] implemented an educational intervention that combined direct face-to-face counseling with a behavioral strategy by providing a medication-taking schedule. This intervention included a modified medication schedule presented in a table format, which illustrated the daily therapy regimen with pictures of the antiepileptic drugs and cues to remind patients to take their medication. This approach helps patients better understand their treatment regimen and prevents them from missing doses. Lastly, Zheng et al. [26] explored the effects of comprehensive counseling provided by multidisciplinary health worker teams.
According to the reviewed studies, interventions conducted by pharmacists have played a crucial role in improving patient health outcomes, particularly in enhancing medication adherence. Research conducted by AlAjmi et al. [7], Fogg et al. [21], Chandrasekhar et al. [27], Jarad et al. [28], and Tamilselvan et al. [29] demonstrates that educational interventions, either through direct verbal counseling or structured 30-minute faceto-face interviews, can significantly increase adherence to medication regimens and strengthen patients’ belief in their treatment (Table 1). Additionally, studies by AlAjmi et al. [7] and Jarad et al. [28] indicated a significant difference in drug adherence between control and intervention groups. Another effective counseling method, providing leaflets, has proven particularly beneficial for caregivers of pediatric epilepsy patients [24]. In the realm of pharmaceutical care, counseling is crucial for enhancing the quality of life among epilepsy patients [36]. The goal of educational interventions is to bolster patient knowledge about the disease and treatment, as well as to alter patient beliefs or perceptions about their treatment, as assessed by a questionnaire. Such education helps reduce patients’ fear of the stigma associated with seizures and enhances their ability to self-manage epilepsy [36]. Educational interventions can be administered by pharmacists or other healthcare professionals, such as doctors. Li et al. [23] developed a program known as the Epilepsy Review Service, which provided comprehensive information about the disease, including the types of seizures, their duration, triggers, and potential side effects. The service also included a therapeutic drug monitoring service, which served as a reference for dose adjustments by prescribing doctors and helps prevent drug toxicity.
Interventions for epilepsy patients can also be administered by a multidisciplinary team of health workers, including pharmacists, neurologists, and nurses. These professionals are expected to deliver integrated and comprehensive information and services tailored to their specific areas of expertise [26]. Such interventions have been shown to significantly enhance medication adherence and quality of life, as measured by the 8-item Morisky Medication Adherence Scale (MMAS-8) and the 31-item Quality of Life in Epilepsy questionnaires, respectively. Moreover, Tang et al. [22] reported that educational interventions (both verbal counseling and written materials) combined with behavioral changes, such as the use of medication reminders, significantly improved medication adherence and seizure control. Patients were prompted to take their medication through the use of illustrated tables that outlined their daily therapy schedules. However, there was no significant difference in outcomes between the control group, which received only educational interventions, and the intervention group, which received both educational and behavioral interventions (Table 2). Behavioral interventions, or skill-based psychological strategies, are implemented to modify behavior. They require practice and understanding to effectively change habits and enhance quality of life [37]. Furthermore, improving patient self-management or self-efficacy in their treatment can lead to greater therapy success, foster adaptation to chronic disease treatment patterns, and directly impact the patient’s quality of life [38].
Adherence to taking medication refers to the extent to which a patient follows the prescriber’s instructions when using medication [6]. Research has shown that adherence to antiepileptic drug therapy can prevent seizures or even achieve seizure freedom in up to 70% of cases [39]. A study by Niriayo et al. [40] found that epilepsy patients with low medication adherence were eleven times more likely to experience uncontrolled seizures compared to those with high medication adherence. Adherence to treatment can be measured directly or indirectly [16]. Direct methods include measuring drug levels in hair or body fluids such as blood or saliva. Indirect methods, in contrast, utilize non-biological tools, including self-reported pill counts, appointment attendance, medication refills, questionnaires, and seizure frequency [41]. Questionnaires are commonly used as indirect measures to assess drug adherence outcomes, including the MMAS-8, MMAS-4 [22,26-28], the Simplified Medication Adherence Questionnaire [25], and the Medication Adherence Report Scale [21].
This scoping review indicates that pharmacists can improve medication adherence and impact other parameters, such as seizure control and quality of life for epilepsy patients, through three types of interventions: educational, psycho-behavioral, and mixed interventions (Table 2). This aligns with findings from a review by Al-Aqeel et al. [32], which suggests that adherence can be increased through these three intervention methods. However, this scoping review has limitations, including only reviewing articles published in English and the need for a broader literature search across more databases. Another limitation is the narrow inclusion criteria related to outcome parameters, as the criteria for this review are limited to pharmaceutical interventions concerning drug use adherence (medication adherence). Future reviews could explore pharmacist interventions on epilepsy awareness, potentially involving other health workers or social workers.
CONCLUSION
Pharmacist interventions have been shown to be effective in improving medication adherence among epilepsy patients. Direct counseling, provided either through face-to-face interactions or digital services, equips patients with essential information about their condition and insights into epilepsy symptoms, seizure triggers, and antiepileptic drugs. Additionally, distributing educational materials like leaflets can be particularly helpful for caregivers of pediatric epilepsy patients. Multidisciplinary interventions that include pharmacists, neurologists, and nurses offer comprehensive care that can improve both drug adherence and the quality of life for epilepsy patients. Furthermore, behavioral interventions, such as medication reminders and skill-based psychological support, can significantly boost medication adherence and seizure control. Overall, pharmacist interventions are crucial in optimizing therapy outcomes, which include increased knowledge of self-management, improved perception of illness, enhanced effectiveness of antiepileptic drugs in controlling seizures, and better quality of life.
Notes
Conflict of Interest
The authors have no conflicts of interest associated with the material presented in this paper.
Funding
This work was supported by the Indonesian Endowment Funds for Education (LPDP) and the Center for Higher Education Funding (BPPT) (No. 202209091837) for financial support for education and research dissertations.
Author Contributions
Conceptualization: Ernawati I, Ikawati Z, Yasin NM, Setyopranoto I. Data curation: Ernawati I, Ikawati Z, Yasin NM, Setyopranoto I. Funding acquisition: Ernawati I. Methodology: Ernawati I, Ikawati Z, Yasin NM, Setyopranoto I. Writing – original draft: Ernawati I, Ikawati Z, Yasin NM, Setyopranoto I. Writing – review & editing: Ernawati I, Ikawati Z, Yasin NM, Setyopranoto I.
Acknowledgements
None.