Articles
- Page Path
- HOME > J Prev Med Public Health > Volume 50(1); 2017 > Article
-
Original Article
Distribution and Determinants of Low Birth Weight in Developing Countries -
Rashidul Alam Mahumud1
 , Marufa Sultana1
, Marufa Sultana1 , Abdur Razzaque Sarker1,2
, Abdur Razzaque Sarker1,2
-
Journal of Preventive Medicine and Public Health 2017;50(1):18-28.
DOI: https://doi.org/10.3961/jpmph.16.087
Published online: December 27, 2016
1Health Economics and Financing Research, Health Systems and Population Studies Division, International Centre for Diarrhoeal Disease Research, Bangladesh (icddr,b), Dhaka, Bangladesh
2Department of Management Science, University of Strathclyde, Glasgow, United Kingdom
- Corresponding author: Rashidul Alam Mahumud, MSc 68 Shaheed Tajuddin Ahmed Sarani, Mohakhali, Dhaka, Bangladesh Tel: +880-2-9827001-10, Fax: +880-2-8811568 E-mail: rashidul.alam@icddrb.org
Copyright © 2017 The Korean Society for Preventive Medicine
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
-
Objectives
- Low birth weight (LBW) is a major public health concern, especially in developing countries, and is frequently related to child morbidity and mortality. This study aimed to identify key determinants that influence the prevalence of LBW in selected developing countries.
-
Methods
- Secondary data analysis was conducted using 10 recent Demography and Health Surveys from developing countries based on the availability of the required information for the years 2010 to 2013. Associations of demographic, socioeconomic, community-based, and individual factors of the mother with LBW in infants were evaluated using multivariate logistic regression analysis.
-
Results
- The overall prevalence of LBW in the study countries was 15.9% (range, 9.0 to 35.1%). The following factors were shown to have a significant association with the risk of having an LBW infant in developing countries: maternal age of 35 to 49 years (adjusted odds ratio [aOR], 1.7; 95% confidence interval [CI], 1.2 to 3.1; p<0.01), inadequate antenatal care (ANC) (aOR, 1.7; 95% CI, 1.1 to 2.8; p<0.01), illiteracy (aOR, 1.5; 95% CI, 1.1 to 2.7; p<0.001), delayed conception (aOR, 1.8; 95% CI, 1.4 to 2.5; p<0.001), low body mass index (aOR, 1.6; 95% CI, 1.2 to 2.1; p<0.001) and being in the poorest socioeconomic stratum (aOR, 1.4; 95% CI, 1.1 to 1.8; p<0.001).
-
Conclusions
- This study demonstrated that delayed conception, advanced maternal age, and inadequate ANC visits had independent effects on the prevalence of LBW. Strategies should be implemented based on these findings with the goal of developing policy options for improving the overall maternal health status in developing countries.
- Infant birth weight is a significant predictor of the immediate and future health status of a newborn. Low birth weight (LBW) is a major public health concern and one of the strongest single risk factors for early neonatal mortality and morbidity [1,2]. According to the World Health Organization, the prevalence of LBW is 15.5% globally, and 96.5% of LBW infants are born in developing countries [3,4]. LBW has been defined as a birth weight of less than 2500 g regardless of gestational age. Consequently, LBW is considered to be associated with a greater risk of early childhood death than is associated with normal birth weight [5]. Furthermore, it is a significant factor associated with higher probabilities of infection, greater susceptibility to childhood illness, lower chances of child survival, long-term physical and mental deficiencies, and problems related to behavior, learning, and psychosocial improvements during childhood [2,6]. In the perinatal period, LBW infants are in a critical state with regard to survival, and approximately half of all neonatal deaths are directly or indirectly linked to LBW [7]. This adverse pregnancy outcome may be influenced by several conditions, such as heart disease, diabetes, hypertension, behavioral disorders, impaired cognitive function, psychological disorders, and a substantial risk of complications related to the stoma includes the esophagus, stomach, duodenum, ileum, colon, pleural cavity, ureters, urinary bladder, and kidney pelvis etc. [8], and usually incurs long-term financial burdens for households [9,10]. Furthermore, with the demographic change of increased life expectancy at birth in developing countries, children born with LBW can cause an increased economic burden and an increased disease burden [10,11]. Consequently, LBW is considered as a universal threat for developing countries that creates a barrier for child development [12,13]. Previous studies have shown several factors to be determinants of LBW and have demonstrated that preventing those factors can help reduce early childhood morbidity and mortality [14]. The determinants of LBW can be broadly classified as genetic, constitutional, obstetric, nutritional, related to maternal morbidities in the antenatal period, toxic exposure-related, and linked to antenatal care (ANC). Other factors including smoking, maternal age, birth spacing, ANC, anemia, genital infections, maternal ill health, and stress have also been reported [15]. Research on the prevalence and determinants of LBW has been conducted using nationwide population-based survey data, with some studies focusing on developing countries. However, most of the multi-country studies were conducted using recalled birth weight data, with mothers reporting information about the size of their newborn baby (e.g., very small, small, normal, large, and very large) from memory, which may have affected the accuracy of the results regarding LBW [16]. This study used a continuous type of birth weight data derived from Demography and Health Surveys (DHSs) among 10 selected developing countries. However, global development has entered a new era, as world leaders have evaluated the achievements of the Millennium Development Goals and adopted the 2030 Agenda for Sustainable Development in the name of Sustainable Development Goals (SDGs). The specific SDGs known as the health goal (goal No. 3) aims to “ensure healthy lives and promote well-being for all at all ages,” with one of the important targets being to ensure universal access to reproductive health care services, including family planning, information and education, and the integration of reproductive health into national strategies and programs. The aim of this study was to investigate the distribution and determinants of LBW in selected developing countries so that policy makers in all countries can design effective plans for building stronger communities, emphasizing a comprehensive approach to reach their objectives, particularly SDG-3.
INTRODUCTION
- Study Design
- Secondary data analysis was carried out using DHS data for the period of 2010 to 2013 from the following least-developed countries as defined by the World Bank: US (2010), Cambodia (2010), Colombia (2010), Indonesia (2012), Jordan (2012), Nepal (2011), Pakistan (2012-2013), Tanzania (2010), Uganda (2011), and Zimbabwe (2010-2011). Moreover, those surveys used continuous of birth weight data, which was another criterion for choosing those countries.
- Data Collection and Sampling Technique
- The DHS collected national-level household-based survey data on birth weight retrospectively from mothers whose youngest child was under five years of age. The DHS used a stratified, two-stage cluster sampling design. The first stage involved selecting samples from a master sampling frame constructed from enumeration, and the second stage involved systematic sampling of the households listed from each cluster, to ensure that adequate numbers of completed individual interviews were obtained. The survey collected data through questionnaire-based face-to-face interviews, for which women of reproductive age (15 to 49 years) were interviewed based on the Measure DHS program model. Each respondent (mother) was asked to provide a detailed birth history for births in the preceding survey. Birth weight was recorded using the metric scale (in grams) in all selected study countries. Details regarding the sample design, specific consent, and data collection procedures have been reported elsewhere, in the DHS reports from the individual countries [17].
- Outcome Variable
- The DHS recorded birth weight data from mothers whose youngest child was less than five years old in the five years preceding the survey using health card records. Entries on health cards were generally completed by a physician or a health worker and given to mothers upon discharge from the health facility (e.g., hospital, clinic or any other healthcare institution). Reporting birth weight information on health cards has been found to be more reliable than obtaining birth weight information through maternal recall [18]. The birth weight information derived from the DHS may include possible misclassifications, as the DHS used the proxy variable of the reported size of the infant at birth, which may lead to potential heaping [18-21]. This study analyzed only the numerical birth weight data contained in the DHS survey for only the most recent children. Finally, birth weight data were classified into two groups: non-LBW (birth weight ≥2500 g) or LBW (birth weight <2500 g). Data from children with a missing birth weight, mothers with twin or multiple pregnancies, and stillbirths were excluded from the analysis.
- Independent Variables
- The study variables were selected based on epidemiological information, prior studies, a review of the relevant published demographic studies, and the available information in the DHS datasets, with a consideration of potential confounders [22-24]. Individual-level factors such as maternal age, the height of the mother, sex of the child, educational status, occupational status, parity, ANC visits, intake of iron during pregnancy, maternal hemoglobin (Hb) levels, and nutritional status, as well as community-level factors, such as wealth status and place of residence, were considered in the study. Maternal age was divided into the categories of ≤19 years, 20-34 years, and 35-49 years, and maternal height was defined as short (≤145 cm), average (146-155 cm), or tall (>155 cm). The sex of the child was recorded as male or female. Education level was defined as no education, primary education, or secondary or higher education, and current occupational status was classified as not working or working. Frequency of ANC visits was defined as inadequate (0 or 1), intermediate (2 or 3), or adequate (4 or more), and parity was classified as first birth, 2-3 births, 4 or more births. Age at first cohabitation was defined as ≤12 years, 13-17 years, or ≥18 years. Whether the mother had taken iron pills during pregnancy was recorded as yes or no. Maternal Hb levels were measured using the HemoCue (HemoCue, Angelholm, Sweden) rapid testing method, and participants were divided based on whether their Hb level was <12.0 g/dL or ≥12.0 g/dL. Height and body weight were obtained from the dataset, and body mass index (BMI) was calculated as the ratio of weight in kilograms to height in meters squared (kg/m2). BMI was further categorized into three groups: low (≤18.5 kg/m2), normal or healthy weight (18.5-24.9 kg/m2) or overweight (BMI >24.9 kg/m2). The DHS applied an asset-based approach to estimate household wealth status, which was measured based on the ownership of durable assets. Each variable (asset) was dichotomized as 1 if present and 0 if not, and the wealth index was constructed using principal component analysis (PCA). Weights were determined by factor scores derived from the first principal component in the PCA. The constructed wealth index values were then assigned to each individual based on common variables. We established cutoff values for percentiles of the population, and we classified participants into three groups: poor (bottom 40%), middle (middle 40%), or rich (top 20%), following the cutoffs used in an earlier study. Place of residence was classified as rural or urban.
- Statistical Analysis
- In the descriptive analyses, the characteristics of the study population for selected countries were expressed as percentages (%) with 95% confidence interval (CIs). For independent variables, the category found to be at the least risk for having an LBW baby in the analysis was considered as the reference for constructing odds ratios (ORs). A multivariate logistic regression model was applied to estimate ORs as a measure of the associations between LBW and related risk factors after considering potential confounders. The diagnostic tests were employed in the analyses. Normality test for the birth weight data was accomplished through graphically. Goodness of fit was assessed using the Hosmer and Lemeshow statistic [25]. The variance inflation factor (VIF) test was performed to determine whether multicollinearity was present. For all the tests conducted in the study, p<0.05 were considered to indicate statistical significance. In the analyses, the sampling weight was adjusted based on the DHS data [26], and all statistical analyses were carried out using Stata/SE 13.0 (StataCorp, College Station, TX, USA).
- Ethical Approval
- Ethical clearance to conduct the DHS was obtained from the Measure DHS and the Ethics Committee of ICF Macro (Calverton, MD, USA). The DHS data are publicly accessible and were made available to us upon request by Measure DHS.
METHODS
- Population Characteristics
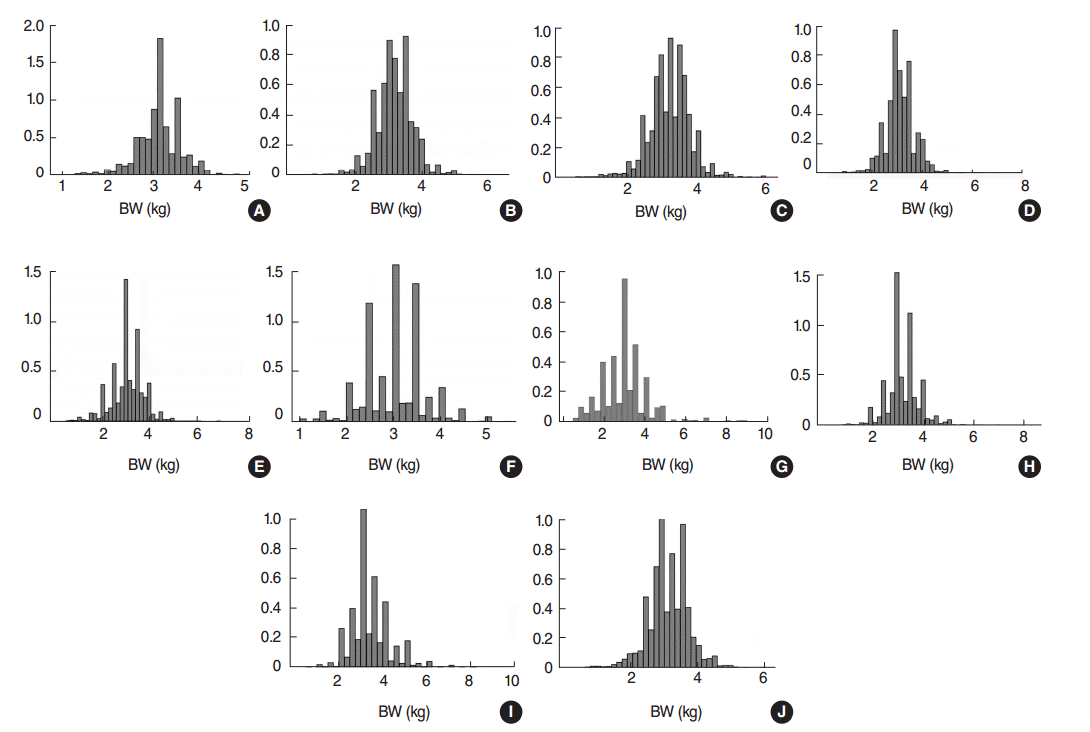
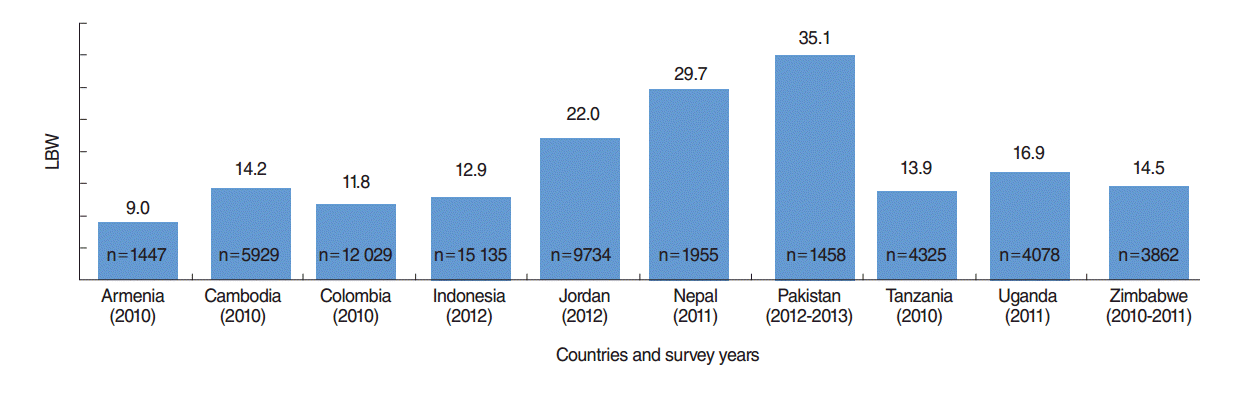
- A total of 59 932 live births were recorded in the study countries (Table 1); Indonesia had the highest number (15 135 live births), followed by Colombia (12 029 live births). Birth weight data were demonstrated to be normally distributed (Figure 1). The overall prevalence of LBW was 15.9% (95% CI, 15.6 to 16.2%), and the average birth weight of LBW babies was 2179 g (Figure 2). Pakistan had the highest prevalence of LBW (35.1%; 95% CI, 32.9 to 37.3%), followed by Nepal (29.7%; 95% CI, 27.7 to 31.7%), with average birth weights of 1988 g and 2255 g, respectively (Table 1).
- The majority of the mothers (73.5%) were between 20 and 34 years of age, and more than half of the mothers did not have any formal education, with the highest proportion found in Pakistan (57.2%), followed by Nepal (46.5%) (Table 2). Overall, 52% of mothers were non-working, with the highest amount observed in Jordan (85.7%), followed by Pakistan (74.2%). Approximately 93.8% of mothers had taken iron pills, and more than 63% of mothers had not an acceptable level of Hb (<12.0 g/dL). Overall, approximately 69.8% of mothers received adequate ANC (4 or more visits) during their last pregnancy. However, the highest percentages of adequate ANC were observed among the mothers in Armenia (94.8%), Colombia (89.8%), Indonesia (88.4%), and Jordan (94.5%). Nearly half of the mothers lived in households with a low socioeconomic status (Table 2).
- Factors Influencing the Determinants of Low Birth Weight
- In this study, step-up methods were used to enter all factors into a single regression model for adjusted analysis (Table 3). This model showed that a number of factors significantly influenced LBW. The regression model explained 22% of total variation (Cox-Snell R2 =22%). The VIF test, which had a mean (maximum) value of 2.22 (4.12), indicated that no evidence of multicollinearity was present in the regression model. The Hosmer and Lemeshow statistic showed no significant difference between the model and observed data, confirming a good fit of the model to the data. Mothers with advanced age (35 to 49 years) had a significantly greater risk of delivering LBW babies than younger mothers (p<0.01) (Table 3). Illiterate mothers (no formal education) had a higher risk of delivering LBW babies than more highly educated mothers in Armenia (OR, 1.4; 95% CI, 1.1 to 2.2; p<0.01), Indonesia (OR, 2.5; 95% CI, 1.5 to 4.4; p<0.001), Jordan (OR, 1.6; 95% CI, 1.1 to 2.7; p<0.01), Nepal (OR, 1.3; 95% CI, 1.1 to 1.5; p<0.001), Pakistan (OR, 2.6; 95% CI, 1.3 to 6.6; p<0.001), and Uganda (OR, 2.1; 95% CI, 1.6 to 7.6; p<0.01). Female babies were more prone to have a LBW than male babies in Armenia (OR, 1.4; 95% CI, 1.1 to 1.8; p<0.01), Cambodia (OR, 1.4; 95% CI, 1.1 to 1.6; p<0.01), Colombia (OR, 1.3; 95% CI, 1.1 to 1.5; p<0.001), Indonesia (OR, 1.2; 95% CI, 1.1 to 1.3; p<0.001), Jordan (OR, 1.6; 95% CI, 1.3 to 1.8; p<0.001), and Tanzania (OR, 1.4; 95% CI, 1.1 to 1.9; p<0.001), as well as in all countries overall (OR, 1.4; 95% CI, 1.3 to 1.6; p<0.001).
- Moreover, delayed conception (over 48 months) had significant relationship with LBW in Armenia (OR, 2.8; 95% CI, 1.6 to 4.1; p<0.01), Cambodia (OR, 1.9; 95% CI, 1.1 to 3.7; p<0.01), Colombia (OR, 1.4; 95% CI, 1.1 to 1.9; p<0.01), Jordan (OR, 2.2; 95% CI, 1.4 to 3.3; p<0.001), Tanzania (OR, 2.4; 95% CI, 1.1 to 5.4; p<0.01), and Uganda (OR, 2.2; 95% CI, 1.2 to 3.5; p<0.001). In all countries, ANC visits were associated with significant reductions in LBW, while receiving inadequate ANC was associated with an elevated risk of LBW (OR, 1.7; 95% CI, 1.1 to 2.8; p<0.01). In addition, in most of the countries, we observed a significantly increased risk of LBW in newborns born to mothers with certain specific characteristics, such as low BMI (OR, 1.6; 95% CI, 1.2 to 2.1; p<0.001) (with normal weight as the reference), primiparity (OR, 1.5; 95% CI, 1.1 to 2.9; p<0.001) (with parity of 4 or above as the reference), residing in rural communities (OR, 1.5; 95% CI, 1.1 to 1.9; p<0.001), as well as lower wealth status of households (OR, 1.4; 95% CI, 1.2 to 1.8; p<0.001) in comparison with the rich group.
RESULTS
- In this study, we identified potential determinants of the prevalence of LBW in developing countries. Our findings demonstrated that advanced maternal age (35 to 49 years), lack of ANC, primiparity, illiteracy, later conception, and being in the poorest socioeconomic stratum were significantly associated with LBW. Previous studies have likewise found that women with advanced maternal age are more likely to give birth to LBW babies [1,2,27-29]. Pregnant women aged ≥35 years are more likely to increase the probability of risk having pregnancy complications compared with younger women, like as, gestational diabetes, placenta praevia, breech presentation, that might be cause of delivering babies with LBW. Women with poor educational status were generally at a higher risk of having an LBW baby than mothers with secondary or higher education. These findings are consistent with those of some previous studies conducted in developing countries [1,30-32]. We found that later conception was associated with a significantly greater risk of LBW. This may be related to age, because increased age is related to common chronic diseases such as arthritis, hypertension, and diabetes prior to pregnancy [27]. However, these findings are in contrast with those of another study conducted in a developing country [31]. The present study also observed an increased risk of LBW among newborns born to mothers with a low BMI in comparison to normal-weight mothers. This finding parallels those of earlier studies conducted in low-middle income countries showing that infants of low-BMI mothers had a significantly higher likelihood of LBW [31,33-36]. Additionally, low socioeconomic status was a risk factor of LBW, confirming the findings of previous studies that the poorest women in developing countries are at a significantly higher risk of delivering LBW infants [32,37].
- The present study found that receiving insufficient ANC was a significant contributor to LBW. Specifically, in women who failed to receive any ANC or had inadequate ANC than recommended, the risk of LBW was higher than in women attending the standard number of ANC visits [38]. Similar results have also been reported in previous studies conducted in developing countries, although the magnitude of risk appears to vary substantially in different settings depending on the ANC system and the degree of attendance [28,31,35,39]. Comparing our findings to those of prior studies, the evidence suggests that the degree of risk may be diluted in settings with a standard frequency of ANC. Women living in rural communities had a greater risk of LBW than urban mothers. Similar results have been found in other studies [1,2,6,35]. Although this study has some strength, such as the large sample size and quality of data, it also has important limitations. The selected countries were found to have a large amount of missing birth weight data. They were also selected to ensure geographical coverage of less developed regions as well as based on the presence of available data related to the study variables. The reported number of home deliveries may have been influenced by social, cultural, and economic factors, and is likely to be country-specific and region-specific, as well as to change over time, and these possibilities were not captured in this analysis. Moreover, the selected DHSs were conducted in different years, which may have resulted in inconsistencies. A high percentage of babies delivered at home had inadequate birth weight measurements, with a large proportion of missing data. Consequently, many samples were excluded from the study. The aggregation of country data into regional summaries by wealth quintile may have caused errors through the combination of wealth quintiles from countries at differing wealth levels. Additional multilevel analysis of existing datasets could provide more detailed information for individual countries on adverse pregnancy outcomes as well as on health-seeking behavior related to maternal and child health.
- In summary, this study identified some significant risk factors with independent effects on the prevalence of LBW in selected developing countries. Among these factors, inadequate ANC, delayed conception, and maternal age had a greater potential effect on birth weight. Improvements in these specific risk factors might have the positive effect in reducing the incidence of LBW. However, interventions to improve the educational levels of women and female children are also important for reducing the prevalence of LBW. Different strategies should be implemented considering the settings of individual countries, with appropriate community-based interventions focusing on these factors so that policy-makers can design effective plans for improving overall maternal and child health in selected developing countries.
DISCUSSION
ACKNOWLEDGEMENTS
-
CONFLICT OF INTEREST
The authors have no conflicts of interest associated with the material presented in this paper.
Notes
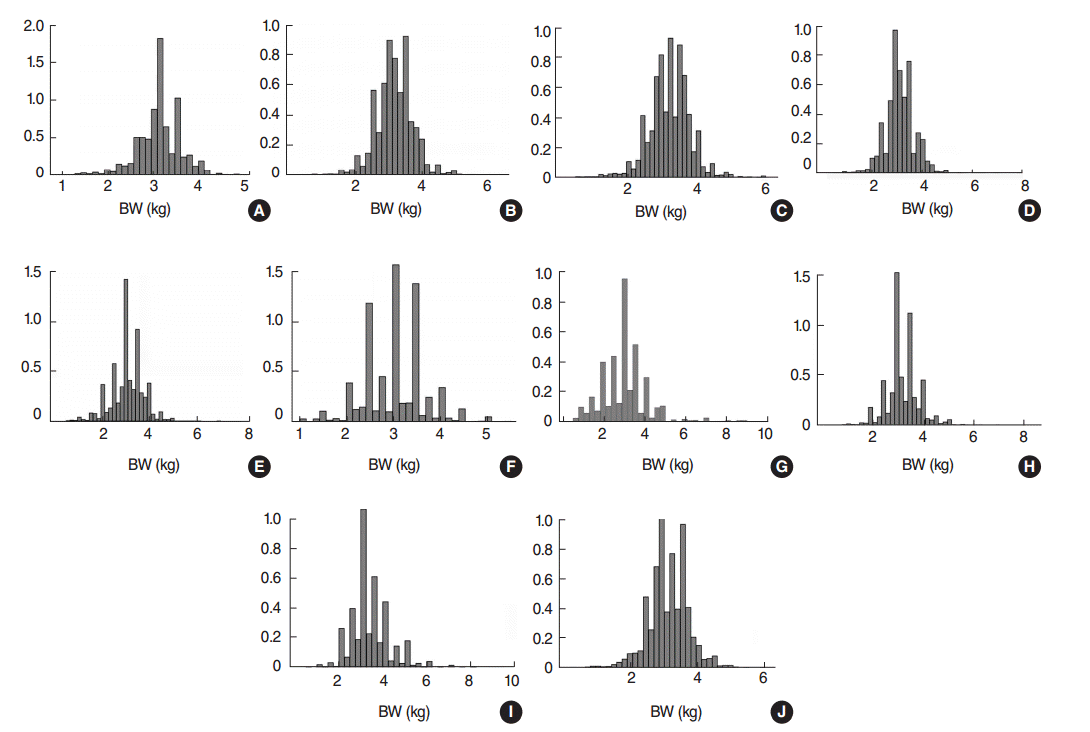
| Countries | Survey years1 | No. of live births2 |
LBW3 |
Extreme LBW4 |
Overall prevalence of LBW5 | ||
|---|---|---|---|---|---|---|---|
| Average weight (g) | Prevalence | Average weight (g) | Prevalence | ||||
| Armenia | 2010 | 1426 | 2214.8 | 8.4 | 1178.6 | 0.5 | 9.0 |
| Cambodia | 2010 | 5929 | 2292.4 | 14.5 | 1085.0 | 0.4 | 14.2 |
| Colombia | 2010 | 12 029 | 2267.8 | 12.2 | 1114.6 | 1.0 | 11.8 |
| Indonesia | 2012 | 15 135 | 2288.7 | 12.2 | 1098.5 | 0.7 | 12.9 |
| Jordan | 2012 | 9734 | 2202.2 | 19.6 | 1036.4 | 1.3 | 22.0 |
| Nepal | 2011 | 1955 | 2294.4 | 27.1 | 1171.1 | 1.0 | 29.7 |
| Pakistan | 2012-2013 | 1458 | 2147.9 | 31.4 | 1079.9 | 5.8 | 35.1 |
| Tanzania | 2010 | 4325 | 2285.8 | 13.0 | 1072.7 | 0.4 | 13.9 |
| Uganda | 2011 | 4078 | 2231.2 | 15.8 | 1012.3 | 0.8 | 16.9 |
| Zimbabwe | 2010-2011 | 3862 | 2270.6 | 14.2 | 1039.3 | 0.8 | 14.5 |
| Total | 59 932 | 2251.7 | 14.9 | 1076.9 | 1.0 | 15.9 | |
LBW, low birth weight; DHS, Demography and Health Survey.
1 All data were derived from the standard DHS.
2 DHS sampling weight was adjusted.
3 LBW was defined as a birth weight between 1500 g and 2500 g.
4 Extreme LBW was defined as a birth weight <1500 g.
5 The overall prevalence of LBW was defined based on an LBW definition of birth weight <2500 g.
| Factors |
Countries |
||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Armenia | Cambodia | Colombia | Indonesia | Jordan | Nepal | Pakistan | Tanzania | Uganda | Zimbabwe | All countries | |
| Constant | 0.4 (0.1, 0.8)** | 0.1 (0.0, 0.2)*** | 0.1 (0.1, 0.4)*** | 0.1 (0.0, 0.2)*** | 0.2 (0.1, 0.4)*** | 0.4 (0.01, 4.7) | 0.02 (0.0, 1.9)* | 0.02 (0.0, 2.2)* | 0.0 (0.0, 0.3)* | 0.1 (0.0, 0.4)*** | 0.6 (0.1, 1.9)*** |
| Maternal age (y) | |||||||||||
| ≤19 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 |
| 20-34 | 0.3 (0.1, 1.1) | 2.0 (0.5, 8.0) | 0.8 (0.6, 1.1) | 0.8 (0.5, 1.2) | 0.5 (0.2, 0.9) | 0.5 (0.2, 1.03) | 9.7 (0.2, 483.4) | 0.6 (0.3, 1.4) | 2.2 (0.2, 19.5) | 0.5 (0.3, 0.8) | 0.7 (0.5, 1.0) |
| 35-49 | 1.6 (1.1, 2.8)* | 3.7 (1.9, 5.3)** | 1.9 (1.6, 3.2)*** | 0.9 (0.6, 1.3) | 1.4 (1.1, 2.8)*** | 1.6 (1.1, 2.5)** | 7.7 (1.2, 14.1)** | 1.4 (1.1, 3.0)** | 1.4 (1.1, 3.9)** | 1.6 (1.1, 2.2)** | 1.7 (1.2, 3.1)** |
| Maternal height (cm) | |||||||||||
| Short (≤ 145) | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 |
| Average (146-155) | NA | 1.5 (0.9, 2.3)** | 2.3 (1.6, 3.1)*** | NA | 1.3 (0.8, 2.2) | 1.1 (0.7, 1.8) | 1.1 (0.3, 3.1) | 1.1 (0.5, 1.9) | 1.2 (0.9, 2.1) | 2.9 (1 , 8.2)* | 1.2 (1.0, 1.6) |
| Tall (>155) | NA | 0.8 (0.6, 0.9)*** | 0.7 (0.6, 0.8)*** | NA | 0.6(0.6, 0.7)*** | 0.8 (0.6, 1.2) | 0.7 (0.5, 0.9)** | 0.7 (0.5, 0.8)*** | 0.5 (0.3, 0.7)*** | 0.8 (0.6 , 0.9)* | 0.7 (0.6, 0.8)*** |
| Sex of child | |||||||||||
| Male | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 |
| Female | 1.4 (1.1, 1.8)** | 1.4 (1.1, 1.6)** | 1.3 (1.1, 1.5)*** | 1.2 (1.1, 1.3)*** | 1.6 (1.3, 1.8)*** | 1.1 (0.7, 1.6) | 1.2 (0.7, 1.7) | 1.4 (1.1, 1.9)*** | 1.2 (0.7, 2.1) | 1.2 (0.7, 2.0) | 1.4 (1.3, 1.6)*** |
| Maternal education | |||||||||||
| No education | 1.4 (1.1, 2.2)** | 0.9 (0.5, 1.8) | 1.3 (0.6, 2.9) | 2.5 (1.5, 4.4)*** | 1.6 (1.1, 2.7)** | 1.3 (1.1, 1.5)*** | 2.6 (1.1, 6.6)*** | 0.6 (0.3, 1.5) | 2.1 (1.1, 7.6)** | 0.8 (0.1, 5.5) | 1.5 (1.1, 2.7)*** |
| Primary | 1.6 (0.6, 4.6) | 1.1 (0.7, 1.8) | 0.9 (0.7, 1.2) | 1.4 (1.2, 1.7)** | 1.4 (1.1, 2.1)* | 1.4 (0.6, 2.2) | 2.8 (1.3, 6.1)*** | 0.6 (0.3, 0.8)* | 0.6 (0.2, 1.5) | 1.1 (0.7, 1.6) | 1.6 (1.2, 1.8)* |
| Secondary or higher | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 |
| Maternal occupation | |||||||||||
| Not working | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 |
| Working | 1.1 (0.5, 2.2) | 1.2 (0.8, 1.7) | 1.0 (0.9, 1.2) | 1.0 (0.9, 1.2) | 0.9 (0.7, 1.3) | 1.5 (1.1, 2.8)** | 1.4 (1.1, 2.7)*** | 0.7 (0.5, 1.2) | 0.9 (0.5, 2.1) | 1.2 (0.8 , 1.6) | 0.8 (0.6, 1.9) |
| Marriage to first birth interval (mo) | |||||||||||
| First birth | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 |
| <24 | 0.5 (0.3, 0.9) | 1.3 (0.9, 2.1) | 1.1 (0.9, 1.4) | 0.8 (0.7, 0.9)* | 1.2 (0.9, 1.5) | 0.9 (0.5, 1.7) | 0.9 (0.4, 1.7) | 0.9 (0.6, 1.6) | 1.8 (0.8, 4.1) | 1.3 (0.8, 1.8) | 1.2 (0.9, 1.4) |
| 24-47 | 1.4 (0.6, 2.9) | 1.2 (0.7, 2.0) | 1.3 (0.9, 1.4) | 0.9 (0.8, 1.2) | 1.1 (0.8, 1.5) | 1.1 (0.5, 2.1) | 1.5 (0.7, 3.1) | 1.3 (0.8, 2.3) | 2.9 (1.2, 7.1) | 1.4 (0.8, 2.4) | 1.2 (0.8, 1.5) |
| ≥ 48 | 2.8 (1.6, 4.1)*** | 1.9 (1.1, 3.7)** | 1.4 (1.1, 1.9)** | 0.9 (0.7, 1.4) | 2.2 (1.4, 3.3)*** | 0.8 (0.3, 2.3) | 0.8 (0.3, 2.3) | 2.4 (1.1, 5.4)** | 2.2 (1.2, 3.5)** | 1.5 (0.6, 3.3) | 1.8 (1.4, 2.5)*** |
| Parity | |||||||||||
| First child | 1.5 (1.1, 2.7)** | 1.3 (0.9, 1.9)** | 1.3 (1.1, 3.2)*** | 1.7 (1.1, 2.9)*** | 1.0 (0.8, 1.3) | 1.4 (1.1, 2.1)** | 1.4 (1.1, 3.1)*** | 1.4 (1.1, 2.8)*** | 1.4 (1.1, 2.9)** | 1.3 (1.0, 1.8)* | 1.5 (1.1, 2.9)*** |
| 2-3 | 1.0 (0.6, 1.5) | 0.8 (0.5, 1.2) | 0.8 (0.7, 0.9) | 0.6 (0.6, 0.7)* | 1.1 (0.9, 1.4) | 0.7 (0.4, 1.2) | 0.7 (0.4, 1.2) | 0.6 (0.4, 0.9) | 0.6 (0.3, 1.3) | 0.7 (0.5, 0.9) | 1.6 (0.3, 2.9) |
| ≥4 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 |
| Took iron pills | |||||||||||
| No | 1.7 (0.8, 4.3) | 2.5 (1.1, 7.5)* | NA | 1.3 (1.1, 1.5)** | 4.4 (3.2, 6.1)*** | 0.2 (0.1, 13.5) | 4.2 (1.8, 9.5)*** | 0.5 (0.1, 3.9) | 0.9 (0.3, 3.2) | NA | 3.0 (2.4, 4.1)*** |
| Yes | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 |
| Maternal anemia (Hb, g/dL) | |||||||||||
| Anemic (<12.0) | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 |
| Non-anemic (≥12.0) | NA | 1.3 (0.9, 1.9) | NA | NA | 0.9 (0.7, 1.1) | 2.0 (1.2, 3.3)*** | NA | 1.2 (0.8, 1.8) | 1.3 (0.5, 2.9) | 0.8 (0.5, 1.1) | 1.0 (0.9 , 1.2) |
| No. of ANC visits | |||||||||||
| Inadequate (0 or 1) | 0.8 (0.2, 5.4) | 1.3 (0.6, 2.7) | 3.4 (2.2, 5.4)** | 2.4 (1.3, 3.4)*** | 3.6 (1.6, 8.1)*** | 1.5 (1.1, 5.9)** | 1.3 (1.1, 1.8)** | 3.6 (1.5, 8.9)*** | 3.2 (1.8, 7.1)*** | 4.9 (2.9, 8.2)*** | 1.7 (1.1, 2.8)** |
| Intermediate (2 or 3) | 3.6 (0.7, 18.4) | 1.1 (0.4, 2.7) | 2.7 (1.7, 4.6)*** | 2.0 (1.2, 3.3)*** | 1.7 (1.1, 4.3)** | 1.7 (0.6, 4.8) | 2.3 (0.6, 9.8) | 2.1 (1.2, 3.1) | 2.3 (0.3, 19.1) | 3.2 (1.4, 7.2)*** | 1.5 (1.1, 2.8)** |
| Adequate (4 or more) | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 |
| Place of delivery | |||||||||||
| Facility | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 |
| Home | NA | 1.2 (0.6, 2.4) | NA | 1.4 (1.1, 2.1)** | NA | 1.4 (1.2, 2.9)** | 1.2 (0.9, 2.9) | 1.5 (1.2, 3.2)* | 1.3 (1.0, 2.9)** | 2.5 (2.1, 3.5)* | 1.6 (1.3, 2.1)** |
| Nutritional status | |||||||||||
| Low BMI | NA | 2.9 (1.4, 6.3)*** | 1.5 (1.1, 2.0)** | NA | 2.2 (1.3, 3.9)*** | 1.9 (1.1, 4.9)** | 1.5 (1.1, 3.1)** | 1.2 (0.9, 2.6)** | 1.9 (1.2, 4.8)** | 1.2 (0.9, 1.9)** | 1.6 (1.2, 2.1)*** |
| Normal BMI | NA | 1.6 (0.8, 3.1) | 0.7 (0.6, 0.8) | NA | 1.3 (1.1, 1.6)** | 1.4 (0.6, 2.9) | 0.7 (0.4, 1.2) | 1.0 (0.6, 1.7) | 2.4 (0.8, 5.5) | 0.9 (0.6, 1.4) | 1.1 (0.9, 1.3) |
| Overweight | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 |
| Wealth status | |||||||||||
| Poor (lower 40%) | 2.0 (1.1, 5.0)* | 1.6 (1.2, 3.2)** | 1.3 (1.1, 1.8)*** | 1.3 (1.1, 1.7)** | 1.7 (1.2, 2.9)** | 1.5 (1.1, 2.3)** | 3.4 (1.9, 7.5)** | 1.4 (1.1, 2.8)* | 0.7 (0.2, 2.6) | 1.3 (1.1, 2.2)** | 1.4 (1.1, 1.8)** |
| Middle (middle 40%) | 1.1 (0.5, 2.3) | 1.2 (0.6, 2.4) | 1.0 (0.8, 1.3) | 1.2 (0.9, 1.5) | 0.9 (0.6, 1.1) | 0.8 (0.4, 1.5) | 0.9 (0.4, 1.7) | 0.8 (0.5, 1.5) | 1.1 (0.3, 3.6) | 1.2 (0.8, 1.8) | 1.0 (0.8, 1.3) |
| Rich (upper 20)% | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 |
| Place of residence | |||||||||||
| Urban | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 |
| Rural | 1.4 (1.1, 1.6)** | 1.5 (1.1, 2.8)** | 1.0 (0.8, 1.8) | 1.3 (1.1, 1.5)** | 1.5 (1.1, 1.9)** | 1.3 (1.1, 2.2)** | 0.9 (0.5, 1.9) | 0.5 (0.3, 0.9)** | 1.1 (0.9, 1.9)** | 0.8 (0.6, 1.3) | 1.5 (1.1, 1.9)** |
| Total (n) | 1426 | 5929 | 12 029 | 15 135 | 9734 | 1955 | 1458 | 4325 | 4078 | 3862 | 59 932 |
| Likelihood ratio chi-square | 31.7** | 82.5*** | 82.8*** | 22.5*** | 149.5*** | 38.3*** | 78.0*** | 29.2*** | 40.8*** | 89.3*** | 212.8*** |
| Cox-Snell R2 (%) | 12.9 | 19.7 | 11.8 | 18.7 | 22.1 | 23.0 | 15.8 | 14.3 | 22.1 | 29.3 | 22.0 |
| Hosmer-Lemeshow statistic | 335.6*** | 293.3** | 792.3*** | 385.7*** | 286.7*** | 163.9*** | 744.3*** | 280.3*** | 254.8*** | 836.4*** | 427.3*** |
| Mean VIF (Max) | 3.2 (4.6) | 2.9 (3.7) | 2.6 (4.6) | 3.2 (3.9) | 3.6 (4.1) | 3.4 (4.3) | 3.1 (4.5) | 3.9 (4.3) | 3.9 (4.6) | 3.9 (4.9) | 2.2 (4.1) |
- 1. Rezende Chrisman J, Mattos IE, Koifman RJ, Koifman S, Moraes Mello Boccolini P, Meyer A. Prevalence of very low birthweight, malformation, and low Apgar score among newborns in Brazil according to maternal urban or rural residence at birth. J Obstet Gynaecol Res 2016;42(5):496-504ArticlePubMed
- 2. Assefa N, Berhane Y, Worku A. Wealth status, mid upper arm circumference (MUAC) and antenatal care (ANC) are determinants for low birth weight in Kersa, Ethiopia. PLoS One 2012;7(6):e39957ArticlePubMedPMC
- 3. Brämer GR. International statistical classification of diseases and related health problems. Tenth revision. World Health Stat Q 1988;41(1):32-36PubMed
- 4. Sachdev HP. Low birth weight in South Asia. Int J Diabetes Dev Ctries 2001;21(1):13-31
- 5. Yadav DK, Chaudhary U, Shrestha N. Risk factors associated with low birth weight. J Nepal Health Res Counc 2011;9(19):159-164PubMed
- 6. Metgud CS, Naik VA, Mallapur MD. Factors affecting birth weight of a newborn--a community based study in rural Karnataka, India. PLoS One 2012;7(7):e40040ArticlePubMedPMC
- 7. Lau C, Ambalavanan N, Chakraborty H, Wingate MS, Carlo WA. Extremely low birth weight and infant mortality rates in the United States. Pediatrics 2013;131(5):855-860ArticlePubMed
- 8. Nose S, Sasaki T, Saka R, Minagawa K, Okuyama H. A sutureless technique using cyanoacrylate adhesives when creating a stoma for extremely low birth weight infants. Springerplus 2016;5: 189ArticlePubMedPMC
- 9. Canadian Institute for Health Information. Giving birth in Canada: the costs. Ottawa: Canadian Institute for Health Information; 2006. p. 1-62
- 10. Hodek JM, von der Schulenburg JM, Mittendorf T. Measuring economic consequences of preterm birth: methodological recommendations for the evaluation of personal burden on children and their caregivers. Health Econ Rev 2011;1(1):6ArticlePubMedPMC
- 11. Barker DJ, Forsén T, Uutela A, Osmond C, Eriksson JG. Size at birth and resilience to effects of poor living conditions in adult life: longitudinal study. BMJ 2001;323(7324):1273-1276ArticlePubMedPMC
- 12. Martinson ML, Reichman NE. Socioeconomic inequalities in low birth weight in the United States, the United Kingdom, Canada, and Australia. Am J Public Health 2016;106(4):748-754ArticlePubMedPMC
- 13. Kalanda B, Verhoeff F, le Cessie S, Brabin J. Low birth weight and fetal anaemia as risk factors for infant morbidity in rural Malawi. Malawi Med J 2009;21(2):69-74ArticlePubMedPMC
- 14. Dasgupta A, Basu R. Determinants of low birth weight in a Block of Hooghly, West Bengal: a multivariate analysis. Int J Biol Med Res 2011;2(4):838-842
- 15. Deshpande JD, Phalke DB, Bangal VB, Peeyuusha D, Sushen B. Maternal risk factors for low birth weight neonates: a hospital based case control study in rural area of western maharashtra, India. Natl J Community Med 2011;2(3):394-398
- 16. Boerma JT, Weinstein KI, Rutstein SO, Sommerfelt AE. Data on birth weight in developing countries: can surveys help? Bull World Health Organ 1996;74(2):209-216PubMedPMC
- 17. ICF International. Survey organization manual for demographic and health surveys. 2012 [cited 2016 Dec 30]. Available from: http://dhsprogram.com/pubs/pdf/DHSM10/DHS6_Survey_Org_Manual_7Dec2012_DHSM10.pdf
- 18. Channon AA, Padmadas SS, McDonald JW. Measuring birth weight in developing countries: does the method of reporting in retrospective surveys matter? Matern Child Health J 2011;15(1):12-18ArticlePubMed
- 19. Robles A, Goldman N. Can accurate data on birthweight be obtained from health interview surveys? Int J Epidemiol 1999;28(5):925-931ArticlePubMed
- 20. Blanc AK, Wardlaw T. Monitoring low birth weight: an evaluation of international estimates and an updated estimation procedure. Bull World Health Organ 2005;83(3):178-185PubMedPMC
- 21. ORC Macro. DHS and World Bank use wealth index to measure socioeconomic status. DHS Dimens 2002;4(2):1-2
- 22. Hazarika I. Factors that determine the use of skilled care during delivery in India: implications for achievement of MDG-5 targets. Matern Child Health J 2011;15(8):1381-1388ArticlePubMed
- 23. West BT. Statistical and methodological issues in the analysis of complex sample survey data: practical guidance for trauma researchers. J Trauma Stress 2008;21(5):440-447ArticlePubMed
- 24. Titaley CR, Dibley MJ, Agho K, Roberts CL, Hall J. Determinants of neonatal mortality in Indonesia. BMC Public Health 2008;8: 232ArticlePubMedPMCPDF
- 25. Hosmer DW, Lemeshow S. Applied logistic regression. 2nd ed. New York: Wiley; 2000. p. 1-383
- 26. Rutstein SO, Rojas G. Guide to DHS statistics: demographic and health surveys methodology. 2006 [cited 2017 Jan 18]. Available from: http://www.dhsprogram.com/pubs/pdf/DHSG1/Guide_to_DHS_Statistics_29Oct2012_DHSG1.pdf
- 27. Dietl A, Cupisti S, Beckmann MW, Schwab M, Zollner U. Pregnancy and obstetrical outcomes in women over 40 years of age. Geburtshilfe Frauenheilkd 2015;75(8):827-832ArticlePubMedPMC
- 28. Isiugo-Abanihe UC, Oke OA. Maternal and environmental factors influencing infant birth weight in Ibadan, Nigeria. Afr Popul Stud 2011;25(2):250-266Article
- 29. Nobile CG, Raffaele G, Altomare C, Pavia M. Influence of maternal and social factors as predictors of low birth weight in Italy. BMC Public Health 2007;7: 192ArticlePubMedPMCPDF
- 30. Muthayya S. Maternal nutrition & low birth weight - what is really important? Indian J Med Res 2009;130(5):600-608PubMed
- 31. Khatun S, Rahman M. Socio-economic determinants of low birth weight in Bangladesh: a multivariate approach. Bangladesh Med Res Counc Bull 2008;34(3):81-86ArticlePubMed
- 32. Sebayang SK, Dibley MJ, Kelly PJ, Shankar AV, Shankar AH; SUMMIT Study Group. Determinants of low birthweight, small-for-gestational-age and preterm birth in Lombok, Indonesia: analyses of the birthweight cohort of the SUMMIT trial. Trop Med Int Health 2012;17(8):938-950ArticlePubMed
- 33. Euser AM, Finken MJ, Keijzer-Veen MG, Hille ET, Wit JM, Dekker FW, et al. Associations between prenatal and infancy weight gain and BMI, fat mass, and fat distribution in young adulthood: a prospective cohort study in males and females born very preterm. Am J Clin Nutr 2005;81(2):480-487ArticlePubMed
- 34. Yazdanpanahi Z, Forouhari S, Parsanezhad ME. Prepregnancy body mass index and gestational weight gain and their association with some pregnancy outcomes. Iran Red Crescent Med J 2008;10(4):326-331
- 35. Kayode GA, Amoakoh-Coleman M, Agyepong IA, Ansah E, Grobbee DE, Klipstein-Grobusch K. Contextual risk factors for low birth weight: a multilevel analysis. PLoS One 2014;9(10):e109333ArticlePubMedPMC
- 36. Ronnenberg AG, Wang X, Xing H, Chen C, Chen D, Guang W, et al. Low preconception body mass index is associated with birth outcome in a prospective cohort of Chinese women. J Nutr 2003;133(11):3449-3455ArticlePubMed
- 37. Olsén P, Vainionpää L, Pääkkö E, Korkman M, Pyhtinen J, Järvelin MR. Psychological findings in preterm children related to neurologic status and magnetic resonance imaging. Pediatrics 1998;102(2 Pt 1):329-336ArticlePubMed
- 38. Tellapragada C, Eshwara VK, Bhat P, Acharya S, Kamath A, Bhat S, et al. Risk factors for preterm birth and low birth weight among pregnant Indian women: a hospital-based prospective study. J Prev Med Public Health 2016;49(3):165-175ArticlePubMedPMCPDF
- 39. Raatikainen K, Heiskanen N, Heinonen S. Under-attending free antenatal care is associated with adverse pregnancy outcomes. BMC Public Health 2007;7: 268ArticlePubMedPMCPDF
REFERENCES
Figure & Data
References
Citations

- Associations of forms of intimate partner violence with low birth weight in India: findings from a population-based Survey
Mostafizur Rahman, Helal Uddin, Lutfun Nahar Lata, Jalal Uddin
The Journal of Maternal-Fetal & Neonatal Medicine.2024; 35(25): 7972. CrossRef - Evaluating causal influence of maternal educational attainment on offspring birthweight via observational study and Mendelian randomization analyses
Yiyang Zhu, Hao Zhang, Jike Qi, Yuxin Liu, Yu Yan, Ting Wang, Ping Zeng
SSM - Population Health.2024; 25: 101587. CrossRef - A cohort study of maternal near-miss events and its adverse perinatal outcomes: an obstetrical finding in Northwest Ethiopia
Besfat Berihun Erega, Wassie Yazie Ferede
AJOG Global Reports.2024; 4(1): 100311. CrossRef - Effect of a chimney-fitted improved stove on pregnancy outcomes in Northwest Ethiopia: a randomized controlled trial
Habtamu Demelash Enyew, Abebe Beyene Hailu, Seid Tiku Mereta
BMC Pregnancy and Childbirth.2024;[Epub] CrossRef - Assessment of iron status and red cell parameters in healthy term small for gestational age neonates at birth
Arif Hossain, Shorna Rahman, Shahana Akter, Ismat Jahan, Sanjoy Kumer Dey, Abdul Mannan, Mohammod Shahidullah
Clinical and Experimental Pediatrics.2024; 67(4): 221. CrossRef - Low birthweight and its associated factors in India: A comparative study of national family health survey from the 4th and 5th rounds
Sadashiva Hegde, JangBahadur Prasad, RajeshwariAnnappa Biradar, AlexMotes Carvalho
Indian Journal of Health Sciences and Biomedical Research (KLEU).2023; 16(3): 347. CrossRef - Adaptation outcomes in climate-vulnerable locations: understanding how short-term climate actions exacerbated existing gender inequities in coastal Bangladesh
Saleh Ahmed, Elizabeth Eklund, Elizabeth Kiester
Journal of Environmental Planning and Management.2023; 66(13): 2691. CrossRef - Bayesian Framework for Causal Inference with Principal Stratification and Clusters
Li He, Yu-Bo Wang, William C. Bridges, Zhulin He, S. Megan Che
Statistics in Biosciences.2023; 15(1): 114. CrossRef - Thinner bodies are preferred in China compared to Britain but are not seen as healthier
Xue Lei, David Perrett
Current Psychology.2023; 42(30): 26857. CrossRef - Longitudinal Sleep Study in Pregnancy: Cohort Profile and Prevalence and Risk Factors for Sleep Symptoms in the First Trimester
Chamara V. Senaratna, Nirmala Priyadarshanie, Sharaine Fernando, Sampatha Goonewardena, Pramodya Piyumanthi, Jennifer Perret, Caroline Lodge, Garun S. Hamilton, Shyamali C. Dharmage
International Journal of Environmental Research and Public Health.2023; 20(3): 2070. CrossRef - Epidemiology of neonatal mortality: a spatial and multilevel analysis of the 2019 mini-Ethiopian demographic and health survey data
Temesgen Worku Gudayu
BMC Pediatrics.2023;[Epub] CrossRef - Maternal risk factors associated with term low birth weight in India: A review
Harsh Vats, Ruchi Saxena, Mohinder P. Sachdeva, Gagandeep K. Walia, Vipin Gupta
Anthropological Review.2023; 85(4): 61. CrossRef - The Association of Periodontal Disease with Low Birth Weight Infants: A Case Control Study
Varda Hussain, Anoosha Waseem, Irtaza Husain, Uzma Waseem, Maliha Shahbaz, Fauzia Qureshi
Maternal and Child Health Journal.2023; 27(5): 926. CrossRef - Identification of anthropometric surrogate measurements and their cut-off points for the detection of low birth weight and premature newborn babies using ROC Analysis
Eskedar Sintayehu, Yitagesu Sintayehu, Abdu Oumer, Anteneh Berhane
Journal of Nutritional Science.2023;[Epub] CrossRef - Factors Influencing Undernutrition among Female Adolescent Students in Darchula District, Nepal
Deepika Giri, Nitaya Vajanapoom, Uma Langkulsen
Nutrients.2023; 15(7): 1699. CrossRef - Association between inadequate prenatal care and low birth weight of newborns in Peru: Evidence from a peruvian demographic and health survey
Brenda Caira-Chuquineyra, Daniel Fernandez-Guzman, Humberto Giraldez-Salazar, Diego Urrunaga-Pastor, Guido Bendezu-Quispe
Heliyon.2023; 9(4): e14667. CrossRef - Prevalence and Determinants of Low Birth Weight in India: Findings From a Nationally Representative Cross-Sectional Survey (2019-21)
Siaa Girotra, Neha Mohan, Mansi Malik, Shubhanjali Roy, Saurav Basu
Cureus.2023;[Epub] CrossRef - Facility-based care for moderately low birthweight infants in India, Malawi, and Tanzania
Katherine E. A. Semrau, Rana R. Mokhtar, Karim Manji, Shivaprasad S. Goudar, Tisungane Mvalo, Christopher R. Sudfeld, Melissa F. Young, Bethany A. Caruso, Christopher P. Duggan, Sarah S. Somji, Anne C. C. Lee, Mohamed Bakari, Kristina Lugangira, Rodrick K
PLOS Global Public Health.2023; 3(4): e0001789. CrossRef - Clinical findings and kidney morphology in chronic kidney disease of unknown cause in India
Julia Wijkström, Kumar Chakravarthy Annadata, Carl‐Gustaf Elinder, Praveen Kumar Kolla, Narayana Rao Sarvepalli, Anneli Ring, Rajendiran Swaminathan, Barathi Gunabooshanam, Magnus Söderberg, Vidhya Venugopal, Annika Wernerson
Journal of Internal Medicine.2023; 294(4): 492. CrossRef - National improvements in quality of prenatal healthcare across states and territories in India from 2006 to 2021: a systematic analysis
Kelly Lin, Ethan Chen, Isobel Taylor, Steven Hunter, Jing Sun
Journal of Public Health.2023;[Epub] CrossRef - Nutritional status of Vietnamese infants assessed by Fenton growth chart and related factors: A cross‐sectional study
Lieu Thu Thi Nguyen, Cuong Danh Tran, Ha Thu Thi Nguyen, Hai Thanh Phan, Linh Thuy Nguyen, Huong Lan Thi Nguyen, Anh Hoai Thi Ta, Chau Quynh Thi Pho, Khanh Nam Do, Anh Kim Dang, Huong Thi Le
Pediatric Investigation.2023; 7(4): 254. CrossRef - The association between timing in pregnancy of drought and excess rainfall, infant sex, and birthweight: Evidence from Nepal
Nadia G. Diamond-Smith, Adrienne Epstein, Marya G. Zlatnik, Emily Treleaven
Environmental Epidemiology.2023; 7(5): e263. CrossRef - Regional with urban–rural variation in low birth weight and its determinants of Indian children: findings from National Family Health Survey 5 data
Ramendra Nath Kundu, Anushka Ghosh, Birshikha Chhetri, Indranil Saha, Md. Golam Hossain, Premananda Bharati
BMC Pregnancy and Childbirth.2023;[Epub] CrossRef - A Comparative Cross-sectional Study on Prevalence of Low Birth Weight and its Anticipated Risk Factors
Assmaa A. Alsamae, Hala A. Elzilal, Eman Alzahrani, Hala M. Abo-Dief, Mujeeb A. Sultan
Global Pediatric Health.2023;[Epub] CrossRef - Development and validation of a nomogram for predicting low birth weight among pregnant women who had antenatal care visits at Debre Markos Comprehensive and Specialized Hospital, Ethiopia
Bezawit Melak Fente, Getayeneh Antehunegn Tesema, Temesgen Worku Gudayu, Mengstu Melkamu Asaye
Frontiers in Medicine.2023;[Epub] CrossRef - Gender differences in survival among low birthweight newborns and infants in sub-Saharan Africa: a systematic review
Akalewold T Gebremeskel, Arone W Fantaye, Lena Faust, Pamela Obegu, Sanni Yaya
International Health.2022; 14(2): 122. CrossRef - Impact of Scaling and Periodontal Treatment during Pregnancy on the Risk of Adverse Birth Outcomes
Jhih-Jhen Chen, Dai-Rong Wu, Wei-Szu Lin, I-Chieh Chen, Jeng-Fen Liu, Hui-Ling Chen, Ching-Heng Lin
Journal of Personalized Medicine.2022; 12(2): 137. CrossRef - Exposure to armed conflict as a factor associated with very low birth weight: Case‐control population study
Ginna Cabra‐Bautista, Claudia Marcela Granados Rugeles, Carlos Fernando Grillo‐Ardila, Fabián Armando Gil Laverde
International Journal of Gynecology & Obstetrics.2022; 158(3): 619. CrossRef - Outcomes and Disease Spectrum of LBW Neonates in a Secondary Health Facility
Rosena Olubanke Oluwafemi, Femi Peter Adesina, Adebola Olutoyin Hassan, Mihajlo Jakovljevic
Journal of Healthcare Engineering.2022; 2022: 1. CrossRef - The intergenerational relationship between conditional cash transfers and newborn health
Andreza Daniela Pontes Lucas, Monaliza de Oliveira Ferreira, Tarcisio Daniel Pontes Lucas, Paola Salari
BMC Public Health.2022;[Epub] CrossRef - Treatment of habitual pregnancy miscarriage of various origins
Ara L. Unanyan, Laura G. Pivazyan, Araksya A. Zakaryan, Archil A. Siordiya, Anatoliy I. Ishchenko
V.F.Snegirev Archives of Obstetrics and Gynecology.2022; 9(1): 13. CrossRef - A CORRELATION STUDY BETWEEN TRANSCUTANEOUS BILIRUBIN AND TOTAL SERUM BILIRUBIN LEVELS AMONG NEONATES
ABHISHEK KUMAR SHARMA, KAPIL DHAWAN, MEENAL MAKKAR, RUCHIRA SHARMA
Asian Journal of Pharmaceutical and Clinical Research.2022; : 15. CrossRef - Determinants of Low Birth Weight in a Tertiary Care Hospital in Eastern India
Ratna Panda, Pratibha Jena, Kabita Chanania, Dattatreya Kar
National Journal of Community Medicine.2022; 13(1): 37. CrossRef - Antenatal care attendance and low birth weight of institutional births in sub-Saharan Africa
Alirah Emmanuel Weyori, Abdul-Aziz Seidu, Richard Gyan Aboagye, Francis Arthur- Holmes, Joshua Okyere, Bright Opoku Ahinkorah
BMC Pregnancy and Childbirth.2022;[Epub] CrossRef - Association between Wood and Other Biomass Fuels and Risk of Low Birthweight in Uganda: A Cross-Sectional Analysis of 2016 Uganda Demographic and Health Survey Data
Joshua Epuitai, Katherine E. Woolley, Suzanne E. Bartington, G. Neil Thomas
International Journal of Environmental Research and Public Health.2022; 19(7): 4377. CrossRef - Neonatal Mortality Rate and Its Determinants: A Community–Based Panel Study in Ethiopia
Kasiye Shiferaw, Bezatu Mengistie, Tesfaye Gobena, Merga Dheresa, Assefa Seme
Frontiers in Pediatrics.2022;[Epub] CrossRef - Predicting risks of low birth weight in Bangladesh with machine learning
S. M. Ashikul Islam Pollob, Md. Menhazul Abedin, Md. Touhidul Islam, Md. Merajul Islam, Md. Maniruzzaman, Enamul Kabir
PLOS ONE.2022; 17(5): e0267190. CrossRef - The Influence of Maternal Factors on Neonatal Intensive Care Unit Admission and In-Hospital Mortality in Premature Newborns from Western Romania: A Population-Based Study
Stelian-Gabriel Ilyes, Veronica Daniela Chiriac, Adrian Gluhovschi, Valcovici Mihaela, George Dahma, Adelina Geanina Mocanu, Radu Neamtu, Carmen Silaghi, Daniela Radu, Elena Bernad, Marius Craina
Medicina.2022; 58(6): 709. CrossRef - Socio-economic and cultural determinants of mothers and fathers for low birth weight newborns in the region of Marrakech (Morocco): A case-control study
Mohamed Elaabsi, Mohamed Loukid, Saloua Lamtali, Gouranga Lal Dasvarma
PLOS ONE.2022; 17(6): e0269832. CrossRef - Household food insecurity and physically demanding work during pregnancy are risk factors for low birth weight in north Shewa zone public hospitals, Central Ethiopia, 2021: a multicenter cross-sectional study
Elias Yadeta Debele, Merga Dheresa, Dawit Tamiru, Tegenu Balcha Wadajo, Kasiye Shiferaw, Lemesa Abdisa Sori, Nega Assefa
BMC Pediatrics.2022;[Epub] CrossRef - Risk factors associated with low birth weight
Jana Diabelková, Kvetoslava Rimárová, Peter Urdzík, Erik Dorko, Andrea Houžvičková, Štefánia Andraščíková, Erik Drabiščák, Gabriela Škrečková
Central European Journal of Public Health.2022; 30(Supplement): S43. CrossRef - Effectiveness of Integrated Maternal Nutrition Intervention Package on Birth Weight in Rwanda
Michael Habtu, Alemayehu Gebremariam Agena, Maryse Umugwaneza, Monica Mochama, Cyprien Munyanshongore
Frontiers in Nutrition.2022;[Epub] CrossRef - Determinants of Low Birth Weight Occurrence in Bahteramas Regional General Hospital, Southeast Sulawesi Province, Indonesia
Yuniar Ayu Permata Sari, Wahiduddin Wahiduddin, Ansariadi Ansariadi, Nadjib Bustan, Syamsiar S. Russeng, Saifuddin Sirajuddin, Eri Wijaya
Open Access Macedonian Journal of Medical Sciences.2022; 10(E): 1107. CrossRef - Gains in body mass and body water in pregnancy and relationships to birth weight of offspring in rural and urban Pune, India
Elaine C. Rush, Lindsay D. Plank, Himangi Lubree, Dattatray S. Bhat, Anjali Ganpule, Chittaranjan S. Yajnik
Journal of Nutritional Science.2022;[Epub] CrossRef - Machine learning algorithms for predicting low birth weight in Ethiopia
Wondesen Teshome Bekele
BMC Medical Informatics and Decision Making.2022;[Epub] CrossRef - Drivers and distribution of the household-level double burden of malnutrition in Bangladesh: analysis of mother–child dyads from a national household survey
Abdur Razzaque Sarker, Zakir Hossain, Alec Morton
Public Health Nutrition.2022; 25(11): 3158. CrossRef - Demographic, socio-economic, obstetric, and behavioral factors associated with small-and large-for-gestational-age from a prospective, population-based pregnancy cohort in rural Nepal: a secondary data analysis
Elizabeth A. Hazel, Diwakar Mohan, Scott Zeger, Luke C. Mullany, James M. Tielsch, Subarna K. Khatry, Seema Subedi, Steven C. LeClerq, Robert E. Black, Joanne Katz
BMC Pregnancy and Childbirth.2022;[Epub] CrossRef - Factors Associated with Low Birthweight in Low-and-Middle Income Countries in South Asia
Ngan Ngo, Jahar Bhowmik, Raaj Kishore Biswas
International Journal of Environmental Research and Public Health.2022; 19(21): 14139. CrossRef - Causal Complexity of Perinatal and Late Neonatal Mortality in the Department of Cauca, Colombia from the Perspective of Systems Thinking
Darío Herrera Murgueitio, Norman D. Maldonado, Julián A. Herrera M
European Journal of Medical and Health Sciences.2022; 4(5): 57. CrossRef - Regular antenatal care visits were associated with low risk of low birth weight among newborns in Rwanda: Evidence from the 2014/2015 Rwanda Demographic Health Survey (RDHS) Data
Emmanuel Biracyaza, Samuel Habimana, Donat Rusengamihigo, Heather Evans
F1000Research.2022; 10: 402. CrossRef - Analysing outlier communities to child birth weight outcomes in Malawi: application of multinomial logistic regression model diagnostics
Natasha Sakala, Tsirizani M. Kaombe
BMC Pediatrics.2022;[Epub] CrossRef - Association of geographic distribution and birth weight with sociodemographic factors of the maternal and newborn child of hilly and mountain regions of eastern Nepal: a cross-sectional study
Bharosha Bhattarai, Sagar Panthi, Gopal Kumar Yadav, Swotantra Gautam, Rochana Acharya, Durga Neupane, Nimesh Khanal, Bharat Khatri, Krishna Neupane, Sugat Adhikari, Nimesh Lageju, Lila Bahadur Basnet, Prajjwal Pyakurel, Shankar Prasad Yadav
BMJ Paediatrics Open.2022; 6(1): e001579. CrossRef - Maternal hemoglobin and risk of low birth weight: A hospital-based cross-sectional study in Nepal
Sandeep Kumar Sah, Dev Ram Sunuwar, Josie R. Baral, Devendra Raj Singh, Narendra Kumar Chaudhary, Geeta Gurung
Heliyon.2022; 8(12): e12174. CrossRef - Study on low birth weight and its associated factors among newborns delivered in a tertiary care hospital of Banda district, Uttar Pradesh
Mohd Maroof, Lal Divakar Singh, Seema Barman, Navin Kumar, Santosh Kumar Barman, Mukesh Yadav
Indian Journal of Community Health.2022; 34(4): 525. CrossRef - Depression during pregnancy and the risk of low birth weight, preterm birth and intrauterine growth restriction- an updated meta-analysis
Upama Ghimire, Shireen Salome Papabathini, Joseph Kawuki, Nathan Obore, Taha Hussein Musa
Early Human Development.2021; 152: 105243. CrossRef - Prevalence of low birth weight and its associated factor at birth in Sub-Saharan Africa: A generalized linear mixed model
Zemenu Tadesse Tessema, Koku Sisay Tamirat, Achamyeleh Birhanu Teshale, Getayeneh Antehunegn Tesema, Clive J. Petry
PLOS ONE.2021; 16(3): e0248417. CrossRef - Newborn Birth Weight and Associated Factors Among Mother-Neonate Pairs in Public Hospitals, North Wollo, Ethiopia
Abate Dargie Wubetu, Yosef Eshetie Amare, Assalif Beyene Haile, Melkam Wagaye Degu
Pediatric Health, Medicine and Therapeutics.2021; Volume 12: 111. CrossRef - Hypertensive Disorders during Pregnancy (HDP), Maternal Characteristics, and Birth Outcomes among Japanese Women: A Hokkaido Study
Kritika Poudel, Sumitaka Kobayashi, Chihiro Miyashita, Atsuko Ikeda-Araki, Naomi Tamura, Yu Ait Bamai, Sachiko Itoh, Keiko Yamazaki, Hideyuki Masuda, Mariko Itoh, Kumiko Ito, Reiko Kishi
International Journal of Environmental Research and Public Health.2021; 18(7): 3342. CrossRef - Smoking Cessation during the Second Half of Pregnancy Prevents Low Birth Weight among Australian Born Babies in Regional New South Wales
Pramesh Raj Ghimire, Julie Mooney, Louise Fox, Lorraine Dubois
International Journal of Environmental Research and Public Health.2021; 18(7): 3417. CrossRef - Factors associated with small- and large-for-gestational-age in socioeconomically vulnerable individuals in the 100 Million Brazilian Cohort
Ila R Falcão, Rita de Cássia Ribeiro-Silva, Marcia Furquim de Almeida, Rosemeire L Fiaccone, Natanael J Silva, Enny S Paixao, Maria Yury Ichihara, Laura C Rodrigues, Mauricio L Barreto
The American Journal of Clinical Nutrition.2021; 114(1): 109. CrossRef - The effect of age at first marriage on the incidence of labor complications and babies with low birth weight in Indonesia
Fajar Maulinda, Dwini Handayani, Turro S. Wongkaren
Child Health Nursing Research.2021; 27(2): 127. CrossRef - Regular antenatal care visits were associated with low risk of low birth weight among newborns in Rwanda: Evidence from the 2014/2015 Rwanda Demographic Health Survey (RDHS) Data
Emmanuel Biracyaza, Samuel Habimana, Donat Rusengamihigo, Heather Evans
F1000Research.2021; 10: 402. CrossRef - Factors associated with birthweight and adverse pregnancy outcomes among children in rural Guinea-Bissau - a prospective observational study
Alexander Dahl Stjernholm, Sanne Marie Thysen, Igualdino Da Silva Borges, Ane Bærent Fisker
BMC Public Health.2021;[Epub] CrossRef - Association between iron and folic acid supplementation and birth weight in Ethiopia: systemic review and meta analysis
Andualem Zenebe, Kaleab Tesfaye Tegegne, Berhanu Bifato, Abiyu Ayalew Assefa
Bulletin of the National Research Centre.2021;[Epub] CrossRef - Estado nutricional e fatores associados ao déficit estatural em crianças menores de cinco anos de comunidades remanescentes de quilombos do Nordeste brasileiro
Félix de Jesus Neves, Aline Alves Ferreira, James R. Welch
Cadernos de Saúde Pública.2021;[Epub] CrossRef - Prevalence of low birth weight and macrosomia estimates based on heaping adjustment method in China
Liping Shen, Jie Wang, Yifan Duan, Zhenyu Yang
Scientific Reports.2021;[Epub] CrossRef - Incidence of low birth weight in Mexico: A descriptive retrospective study from 2008–2017
Mónica Ancira-Moreno, Eric Monterrubio-Flores, Sonia Hernández-Cordero, Isabel Omaña-Guzmán, Isidro Soloaga, Fabián Torres, Moisés Reyes, Yohali Burrola-Mendez, Ariana Morales-López, Andrew Amos Channon
PLOS ONE.2021; 16(9): e0256518. CrossRef - Low birth weight and birth weight status in Bangladesh: A systematic review and metaanalysis
Saijuddin Shaikh, Md. Tanvir Islam, Rebecca K. Campbell
Anthropological Review.2021; 84(3): 257. CrossRef - Determinants of Low Birth Weight Among Women Who Gave Birth at Public Health Facilities in North Shewa Zone: Unmatched Case-Control Study
Berhanu Senbeta Deriba, Kemal Jemal
INQUIRY: The Journal of Health Care Organization, Provision, and Financing.2021; 58: 004695802110471. CrossRef - A longitudinal study on the effects of previous stillbirth or abortion on subsequent pregnancies and infants
Berhanu Elfu Feleke, Teferi Elfu Feleke
European Journal of Public Health.2021; 31(6): 1237. CrossRef - Periodontite materna e baixo peso ao nascer: revisão sistemática e metanálise
Edla Carvalho Lima Porto, Isaac Suzart Gomes Filho, Josicélia Estrela Tuy Batista, Amanda Oliveira Lyrio, Elivan Silva Souza, Ana Claudia Morais Godoy Figueiredo, Mauricio Gomes Pereira, Simone Seixas da Cruz
Ciência & Saúde Coletiva.2021; 26( suppl 3): 5383. CrossRef - Determinants of low birth weight and its relationship with stunted toddler status in Magelang Regency, Indonesia
Sri Rum Giyarsih, Ratih Fitria Putri, Agustinur Saputri, Esti Nugraheni, Nia Setiyawati, R. Che Omar, J.T. Sri Sumantyo, B. White, A. Cardenas Tristan, E. Haryono, D.R. Hizbaron, R.F. Putri
E3S Web of Conferences.2021; 325: 06004. CrossRef - Mixed-methods, descriptive and observational cohort study examining feeding and growth patterns among low birthweight infants in India, Malawi and Tanzania: the LIFE study protocol
Linda Vesel, Lauren Spigel, Jnanindra Nath Behera, Roopa M Bellad, Leena Das, Sangappa Dhaded, Shivaprasad S Goudar, Gowdar Guruprasad, Sujata Misra, Sanghamitra Panda, Latha G Shamanur, Sunil S Vernekar, Irving F Hoffman, Tisungane Mvalo, Melda Phiri, Fr
BMJ Open.2021; 11(12): e048216. CrossRef - Inequality of childhood undernutrition in Bangladesh: A decomposition approach
Abdur Razzaque Sarker, Marufa Sultana, Nurnabi Sheikh, Raisul Akram, Nausad Ali, Rashidul Alam Mahumud, Khorshed Alam, Alec Morton
The International Journal of Health Planning and Management.2020; 35(2): 441. CrossRef - Determinants of low birth weight in India: An investigation from the National Family Health Survey
Nizamuddin Khan, Arupendra Mozumdar, Supreet Kaur
American Journal of Human Biology.2020;[Epub] CrossRef - Comparison of therapeutic interventions for recurrent pregnancy loss in association with antiphospholipid syndrome: A systematic review and network meta‐analysis
Xiang Liu, Yuxuan Qiu, Esther Dawen Yu, Shang Xiang, Rui Meng, Kai fan Niu, Huili Zhu
American Journal of Reproductive Immunology.2020;[Epub] CrossRef - Factors Associated with Preterm Birth and Low Birth Weight in Abu Dhabi, the United Arab Emirates
Zainab Taha, Ahmed Ali Hassan, Ludmilla Wikkeling-Scott, Dimitrios Papandreou
International Journal of Environmental Research and Public Health.2020; 17(4): 1382. CrossRef - Evolutionary Strategies for Body Size
Michael A. Little
Frontiers in Endocrinology.2020;[Epub] CrossRef - Association of maternal determinants with low birth weight babies in tea garden workers of Assam
Shashi Nandar Kumar, Sheikh Raisuddin, Kh. Jitenkumar Singh, Banajit Bastia, Deepa Borgohain, Long Teron, Santanu Kumar Sharma, Arun Kumar Jain
Journal of Obstetrics and Gynaecology Research.2020; 46(5): 715. CrossRef - Predictors of Low Birth Weight at Lumbini Provincial Hospital, Nepal: A Hospital-Based Unmatched Case Control Study
Saneep Shrestha, Sandeep Shrestha, Upasana Shakya Shrestha, Kamala Gyawali
Advances in Preventive Medicine.2020; 2020: 1. CrossRef - Wealth-related inequalities of women’s knowledge of cervical cancer screening and service utilisation in 18 resource-constrained countries: evidence from a pooled decomposition analysis
Rashidul Alam Mahumud, Syed Afroz Keramat, Gail M Ormsby, Marufa Sultana, Lal B. Rawal, Khorshed Alam, Jeff Gow, Andre M. N. Renzaho
International Journal for Equity in Health.2020;[Epub] CrossRef - Determinants of Low Birth Weight among Newborns Delivered at Public Hospitals in Sidama Zone, South Ethiopia: Unmatched Case-Control Study
Muse Bututa Bekela, Mulugeta Shegaze Shimbre, Teshale Fikadu Gebabo, Mengesha Boko Geta, Abayneh Tunje Tonga, Eshetu Andarge Zeleke, Negussie Boti Sidemo, Agegnehu Bante Getnet
Journal of Pregnancy.2020; 2020: 1. CrossRef - Epidemiology of low birth weight in Iran: A systematic review and meta-analysis
Mehdi Shokri, Parviz Karimi, Hadis Zamanifar, Fatemeh Kazemi, Milad Azami, Gholamreza Badfar
Heliyon.2020; 6(5): e03787. CrossRef - Social inequalities in low birthweight outcomes in Sri Lanka: evidence from the Demographic and Health Survey 2016
Gayathri Abeywickrama, Sabu S Padmadas, Andrew Hinde
BMJ Open.2020; 10(5): e037223. CrossRef - Development and Validation of a Risk Score to Predict Low Birthweight Using Characteristics of the Mother: Analysis from BUNMAP Cohort in Ethiopia
Hamid Y. Hassen, Seifu H. Gebreyesus, Bilal S. Endris, Meselech A. Roro, Jean-Pierre Van Geertruyden
Journal of Clinical Medicine.2020; 9(5): 1587. CrossRef - Adverse fetal outcomes and its associated factors in Ethiopia: a systematic review and meta-analysis
Getnet Gedefaw, Birhan Alemnew, Asmamaw Demis
BMC Pediatrics.2020;[Epub] CrossRef - Wealth stratified inequalities in service utilisation of breast cancer screening across the geographical regions: a pooled decomposition analysis
Rashidul Alam Mahumud, Khorshed Alam, Syed Afroz Keramat, Andre M. N. Renzaho, Md. Golam Hossain, Rezwanul Haque, Gail M. Ormsby, Jeff Dunn, Jeff Gow
Archives of Public Health.2020;[Epub] CrossRef - Prenatal Mercury Exposure in Pregnant Women from Suriname’s Interior and Its Effects on Birth Outcomes
Gaitree K. Baldewsingh, Jeffrey K. Wickliffe, Edward D. van Eer, Arti Shankar, Ashna D. Hindori-Mohangoo, Emily W. Harville, Hannah H. Covert, Lizheng Shi, Maureen Y. Lichtveld, Wilco C.W.R. Zijlmans
International Journal of Environmental Research and Public Health.2020; 17(11): 4032. CrossRef - Level of physical activity and other maternal characteristics during the third trimester of pregnancy and its association with birthweight at term in South Ethiopia: A prospective cohort study
Meseret Legesse, Jemal Haider Ali, Md Dilshad Manzar, Mohammed Salahuddin, Hamid Yimam Hassen, Frank T. Spradley
PLOS ONE.2020; 15(7): e0236136. CrossRef - Determinants of low birth weight among live birth newborns delivered at public hospitals in Gamo Gofa Zone, South Ethiopia: Unmatched case control study
Alemu Basazin Mingude, Woiynshet Gebretsadik, Dresilgn Misker, Gashaw Garedew Woldeamanuel
SAGE Open Medicine.2020; 8: 205031212094054. CrossRef - Association does not imply prediction: the accuracy of birthweight in predicting child mortality and anthropometric failure
Akshay Swaminathan, Rockli Kim, S.V. Subramanian
Annals of Epidemiology.2020; 50: 7. CrossRef - Factors associated with low birth weight at term: a population-based linkage study of the 100 million Brazilian cohort
Ila R. Falcão, Rita de Cássia Ribeiro-Silva, Marcia F. de Almeida, Rosemeire L. Fiaccone, Aline dos S. Rocha, Naiá Ortelan, Natanael J. Silva, Enny S. Paixao, Maria Yury Ichihara, Laura C. Rodrigues, Mauricio L. Barreto
BMC Pregnancy and Childbirth.2020;[Epub] CrossRef - Prevalence and Determinants of Low Birth Weight in Ethiopia: A Systematic Review and Meta-Analysis
Nuradin Abusha Katiso, Getachew Mullu Kassa, Gedefaw Abeje Fekadu, Abadi Kidanemariam Berhe, Achenef Asmamaw Muche
Advances in Public Health.2020; 2020: 1. CrossRef - Socioeconomic and demographic factors associated with low birth weight in Nepal: Data from 2016 Nepal demographic and health survey
Benojir Ahammed, Md Maniruzzaman, Farzana Ferdausi, MdMenhazul Abedin, MdTanvir Hossain
Social Health and Behavior.2020; 3(4): 158. CrossRef - Maternal exposure to Wenchuan earthquake and prolonged risk of offspring birth outcomes: a natural experiment study
Qiguo Lian, Jiaying Ni, Jun Zhang, Julian Little, Shan Luo, Lin Zhang
BMC Pregnancy and Childbirth.2020;[Epub] CrossRef - Exploring the association between adverse maternal circumstances and low birth weight in neonates: a nationwide population-based study in Bangladesh
Md Mostaured Ali Khan, Md Golam Mustagir, Md Rafiqul Islam, Md Sharif Kaikobad, Hafiz TA Khan
BMJ Open.2020; 10(10): e036162. CrossRef - Regional trends in birth weight in low- and middle-income countries 2013–2018
Irene Marete, Osayame Ekhaguere, Carla M. Bann, Sherri L. Bucher, Paul Nyongesa, Archana B. Patel, Patricia L. Hibberd, Sarah Saleem, Robert L. Goldenberg, Shivaprasad S. Goudar, Richard J. Derman, Ana L. Garces, Nancy F. Krebs, Elwyn Chomba, Waldemar A.
Reproductive Health.2020;[Epub] CrossRef - Modeling the Effect of Mother's Characteristics on the Weight of a Newborn
Oluwafemi Samson Balogun, Donald Douglas Atsa'am, Toluwalase Janet Akingbade, Emmanuel Awuni Kolog, Richard O. Agjei, Samuel Nii Odoi Devine
International Journal of Childbirth.2020; 10(4): 206. CrossRef - Maternal determinants of low birth weight among Indian children: Evidence from the National Family Health Survey-4, 2015-16
Ankita Zaveri, Pintu Paul, Jay Saha, Bikash Barman, Pradip Chouhan, William Joe
PLOS ONE.2020; 15(12): e0244562. CrossRef - Risk of low birth weight and exposure to type of cooking fuel in India
Shekhar Chauhan , Ratna Patel
International Journal of Pregnancy & Child Birth.2020; 6(1): 8. CrossRef - Maternal dietary patterns and risk of adverse pregnancy (hypertensive disorders of pregnancy and gestational diabetes mellitus) and birth (preterm birth and low birth weight) outcomes: a systematic review and meta-analysis
Kelemu Tilahun Kibret, Catherine Chojenta, Ellie Gresham, Teketo K Tegegne, Deborah Loxton
Public Health Nutrition.2019; 22(3): 506. CrossRef - Early Identification of Preterm Neonates at Birth With a Tablet App for the Simplified Gestational Age Score (T-SGAS) When Ultrasound Gestational Age Dating Is Unavailable: Protocol for a Validation Study
Archana B Patel, Kunal Kurhe, Amber Prakash, Savita Bhargav, Suchita Parepalli, Elizabeth V Fogleman, Janet L Moore, Dennis D Wallace, Hemant Kulkarni, Patricia L Hibberd
JMIR Research Protocols.2019; 8(3): e11913. CrossRef - Spatial smoothing of low birth weight rate in Bangladesh using Bayesian hierarchical model
Mohammad Samsul Alam, Syed Shahadat Hossain, Farha Ferdous Sheela
Journal of Applied Statistics.2019; 46(10): 1870. CrossRef - Determinants and adverse perinatal outcomes of low birth weight newborns delivered in Hawassa University Comprehensive Specialized Hospital, Ethiopia: a cohort study
Melaku Desta, Mesfin Tadese, Bekalu Kassie, Mihrete Gedefaw
BMC Research Notes.2019;[Epub] CrossRef - Risk factors for low birth weight in hospitals of North Wello zone, Ethiopia: A case-control study
Tesfahun Mulatu Wachamo, Nigus Bililign Yimer, Asmamaw Demis Bizuneh, Eduardo Ortiz-Panozo
PLOS ONE.2019; 14(3): e0213054. CrossRef - How does birth weight affect health and human capital? A short‐ and long‐term evaluation
Marie Baguet, Christelle Dumas
Health Economics.2019; 28(5): 597. CrossRef - Maternal and early‐life area‐level characteristics and childhood adiposity: A systematic review
Sam Wilding, Nida Ziauddeen, Dianna Smith, Paul Roderick, Nisreen A. Alwan
Obesity Reviews.2019; 20(8): 1093. CrossRef - The Relationship Between Food Insecurity and Anthropometric Measures at Birth in Low Income Households
Asieh Ahmadihoseini, Nasrin Omidvar, Mohsen Nematy, Mohammad Safarian, Maryam Salehi
Iranian Journal of Pediatrics.2019;[Epub] CrossRef - Magnitude of low birth weight and maternal risk factors among women who delivered in Debre Tabor Hospital, Amhara Region, Ethiopia: a facility based cross-sectional study
Maru Mekie, Wubet Taklual
Italian Journal of Pediatrics.2019;[Epub] CrossRef - Measuring perinatal and postpartum quality of life of women and associated factors in semi-urban Bangladesh
Rashidul Alam Mahumud, Nausad Ali, Nurnabi Sheikh, Raisul Akram, Khorshed Alam, Jeff Gow, Abdur Razzaque Sarker, Marufa Sultana
Quality of Life Research.2019; 28(11): 2989. CrossRef - Assessing the impact of antenatal care utilization on low birthweight in India: Analysis of the 2015–2016 National Family Health Survey
Pintu Paul, Ankita Zaveri, Pradip Chouhan
Children and Youth Services Review.2019; 106: 104459. CrossRef - Low birth weight: prevalence and associated factors among newborns at hospitals in Kambata-Tembaro zone, southern Ethiopia 2018
Abebe Alemu, Mulatu Abageda, Biruk Assefa, Getnet Melaku
Pan African Medical Journal.2019;[Epub] CrossRef - Factors associated with low birth weight in Afghanistan: a cross-sectional analysis of the demographic and health survey 2015
Rajat Das Gupta, Krystal Swasey, Vanessa Burrowes, Mohammad Rashidul Hashan, Gulam Muhammed Al Kibria
BMJ Open.2019; 9(5): e025715. CrossRef - Adolescent mothers’ anthropometrics and grandmothers’ schooling predict infant anthropometrics in Ethiopia, India, Peru, and Vietnam
Whitney Schott, Elisabetta Aurino, Mary E. Penny, Jere R. Behrman
Annals of the New York Academy of Sciences.2018; 1416(1): 86. CrossRef - Determinants of low birth weight among neonates born in Amhara Regional State Referral Hospitals of Ethiopia: unmatched case control study
Getnet Asmare, Nigusie Berhan, Mengistu Berhanu, Animut Alebel
BMC Research Notes.2018;[Epub] CrossRef - Both maternal and paternal risk factors for term singleton low birthweight infants in rural Chinese population: a population-based, retrospective cohort study
Shi Chen, Yingying Yang, Yimin Qu, Yun Zou, Huijuan Zhu, Hongbo Yang, Fengying Gong, Linjie Wang, Yu Jiang, Bill Q. Lian, Cynthia Liu, Chengsheng Yan, Jianqiang Li, Qing Wang, Shi-kun Zhang, Hui Pan
Scientific Reports.2018;[Epub] CrossRef - Maternal stress and early-onset colorectal cancer
Qi Zhang, Franklin G. Berger, Bryan Love, Carolyn E. Banister, Elizabeth A. Murphy, Lorne J. Hofseth
Medical Hypotheses.2018; 121: 152. CrossRef - Pre-pregnancy body mass index (BMI) and maternal gestational weight gain are positively associated with birth outcomes in rural Malawi
Austrida Gondwe, Per Ashorn, Ulla Ashorn, Kathryn G. Dewey, Kenneth Maleta, Minyanga Nkhoma, John Mbotwa, Josh M. Jorgensen, Jacobus P. van Wouwe
PLOS ONE.2018; 13(10): e0206035. CrossRef - Low birth weight of institutional births in Cambodia: Analysis of the Demographic and Health Surveys 2010-2014
Chhorvann Chhea, Por Ir, Heng Sopheab, Shyam Sundar Budhathoki
PLOS ONE.2018; 13(11): e0207021. CrossRef - Low birth weight and its associated factors in Ethiopia: a systematic review and meta-analysis
Aklilu Endalamaw, Eshetu Haileselassie Engeda, Daniale Tekelia Ekubagewargies, Getaneh Mulualem Belay, Mekuriaw Alemayehu Tefera
Italian Journal of Pediatrics.2018;[Epub] CrossRef - Determinants of low birth weight in public health facilities, of Kambata Tembaro zone, South Ethiopia
Simegn Alemu, Abdulhalik Workicho, Mamo Nigatu, Tariku Bokila, Tsedeke Wolde
PONS - medicinski casopis.2018; 15(2): 66. CrossRef - The Effect of Moringa-Based Supplementation on Fetal Birth Weight in Jeneponto Regency
Andi Imam Arundhana , Muhammad Syafruddin Nurdin , Veni Hadju , Ansariadi , Andi Zulkifli
Journal of Pharmacy and Nutrition Sciences .2018; 8(3): 144. CrossRef - The Highs and Lows of Fetal Programming for Fatty Liver Disease
Marialena Mouzaki, Simon C. Ling
The Journal of Pediatrics.2017; 187: 13. CrossRef
 KSPM
KSPM

 PubReader
PubReader ePub Link
ePub Link Cite
Cite